- Gounder Gives Lowdown on Ebola, Peptides, and Colorectal Screenings
- ASCO: Pfizer one-ups J&J with Talzenna combo's broad castration-sensitive prostate cancer win
- ASCO: With bispecifics on its heels, Incyte positions Monjuvi combo for first-line DLBCL
- 6 dental technology updates in May
- From clinician to leader: Building confidence, capability and leadership in dentistry
- Operationalizing AI at scale: A practical framework for enterprise-scale success
- 3 key stats on the orthodontist workforce
- Meet the COOs of 10 specialty DSOs
- Data, cross-training, and pipeline development: How health systems are rethinking OR staffing
- How top health systems are redefining the digital patient experience
- ‘The most significant change in 20 years’: Cancer centers prepare for daraxonrasib demand
- A Smooth Handoff From Decision to Dollars: Connecting the Last Mile in Healthcare Payments
- Budget-Strapped Montana Will Stress-Test Trump’s Medicaid Work Rules
- How CEOs actually use hospital rankings — and when they don’t
- What OU Health’s founding CEO learned building a new health system
- Arkansas hospital CEO to step down after 11 years for new role
- The behavioral health workforce pipeline: Where it stands and where it’s headed
- 6 major investments in youth behavioral health
- Coalition for Health AI unveils governance playbook for systems
- 66 health systems ranked by long-term debt
- UnitedHealthcare drops some prior auth requirements for cardiology, orthopedic services
- 8 No Surprises Act shake-ups physicians need to know
- The ASC independence playbook: 3 leaders’ thoughts
- Dr. Rahimah Maina opens new dental practice
- GWU offloaded its $450M physician group problem — why the industry watching
- The gastroenterologist pay gap
- Texas surgery center to double in size, add 2 ORs
- What dental leaders told us in May
- Climate Change: Statement on Proposed Rescission of Climate-Related Disclosure Rules
- Kenyan Court Blocks Trump's Plan To Quarantine Ebola Patients
- What’s going on at the FTC? 3 notes for ASC leaders
- 8 DSOs making headlines
- The physician noncompete battle in 5 key figures
- The physician red flags that can predict a bad ASC partner
- Patient death draws renewed CMS scrutiny at HCA’s Mission Hospital
- Nearly 70% of US counties lack a GI: 13 concerning workforce stats
- Statement of Commissioner Mark T. Uyeda on the Rescission of Climate-Related Disclosure Rules
- A new behavioral health profession is born
- Keynote Remarks at the 2026 Reagan National Economic Forum
- Statement on Proposing Release for Rescission of Climate-Related Disclosure Rules
- Dentists’ pay climbed the most in these 10 states
- Mental Health Disorders Now No. 1 Cause of Disability Worldwide
- Massachusetts AG sues UnitedHealthcare over alleged Medicaid fraud
- UnitedHealthcare to nix nearly two thirds of pediatric prior auths
- Industry Voices—Patients are building a new healthcare system. The industry is finally catching up
- Weekly Rundown—Moffitt Cancer Center expands Reimagine Care's virtual oncology model; Tanner Health deploys AI workforce solution
- Study: LA Canine Outbreak Caused By Low Vaccination Rates, Crowded Boarding
- Ocrelizumab Effective In Slowing Progressive MS, Trial Shows
- Long COVID Might Be Twice As Common As Previously Thought
- In Vaccine-Skeptical California County, A Potential Playbook To Contain Measles
- Heavy Drinking Harms College Students' Brain Power, Study Finds
- A Trump Stronghold Grapples With Health Risks of ICE Detention Sites
- After Her Bout of Amnesia, a $59,000 Billing Dispute Wouldn’t Go Away
- Pharma urged to modernize patient support as young adult cancer rates rise
- Philips adds a spoonful of Disney sugar to ease kids’ MRI anxieties
- MannKind seeks long-awaited sales boost with inhaled insulin approval for kids
- Aetna to launch ‘on demand’ virtual mental health services in 2027
- U of Connecticut dental school reappoints dean for 2nd term
- Michigan dentist charged with Medicaid fraud
- Brand-name drug prices climb after launch in US, fall abroad amid MFN push: report
- ASCO: After Takeda’s defeat, Dizal picks up baton to take on J&J in EGFR lung cancer subtype
- Acadia in the headlines: 6 things to know
- 26 behavioral health executive moves to know
- AstraZeneca gains 2nd bladder cancer nod in key expansion for Imfinzi
- Advocate Health grows Q1 revenue by 10.8% amid higher volumes, greater efficiency
- Behavioral health hospital operator to pay $32M in Medicare fraud settlement
- Bangladesh Measles Surge Kills 500+ Children; Vaccine Delays Blamed
- Care navigation startup Garner Health banks $100M series E at $2.74B valuation
- HCA bolsters workforce pipeline with healthcare professional college acquisition
- Plant-Based Diet May Cut Obesity Risk For Women In Menopause
- Pharma leaders meet with PM Takaichi in push for Japan to retain R&D edge
- Penn Medicine, K Health partner to deploy AI clinical agents
- CVS restores coverage of Eli Lilly obesity med Zepbound, adds new pill Foundayo
- CVS restores coverage of Eli Lilly obesity med Zepbound, adds new pill Foundayo
- CMS finalizes changes to No Surprises Act dispute resolution process
- Smartwatch App Accurately Detects Major Epileptic Seizures
- Racial Gap Exists For Asthma Inhaler Use
- New Colon Cancer Screening Guidelines Add Blood And At-Home Tests
- Fierce Pharma Asia—More China biotech hawkishness; Pfizer’s $10B Innovent deal; Astellas’ roadmap
- CVS expands partnership with Salesforce for greater call center personalization
- Nurse Convicted In Patient's Death Turns Fatal Drug Error Into Cautionary Tale
- Wearable Ultrasound Patch Monitors High-Risk Pregnancies In Real Time
- In a Vaccine-Skeptical California County, a Potential Playbook To Contain Measles
- Listen to the Latest ‘KFF Health News Minute’
- Teladoc Health inks partnership with Walmart to expand virtual care services
- PharmaEssentia taps Incyte alum Eric Vogel as it eyes Besremi expansion
- Kaléo speaks up on allergy awareness to amplify patient stories
- Privacy and PetShops: Remarks at the Regulatory PETshop Series: Cryptographic Technologies and Financial Services Regulation
- NYC Health + Hospitals adds 2nd behavioral health housing site
- Mindfulness isn’t a perk anymore — it’s a workforce strategy
- With Elahere building steam, AbbVie nets FDA nod for another ImmunoGen cancer asset
- Hospitals again ask FTC, DOJ for exemption from expanded premerger notification filings
- Coalition for Health AI unveils governance playbooks for responsible AI adoption
- Amazon taps Roy Schoenberg to lead healthcare business as Neil Lindsay plans to step down
- Viridian, awaiting FDA decision, taps WuXi Bio in eye drug supply deal
- U.S. To Keep Ebola-Exposed Citizens In Kenya Under New Policy
- CAT on a Hot Tin Roof
- GLP-1 Meds May Help Slow the Spread of Certain Obesity-Related Cancers
- GoodRx launches subscription program for low-cost generic medications, telehealth services
- George Washington University locks deal to hand off debt-ridden physician practice to UHS
- Humana invests $83M in new Florida pharmacy distribution center
- As J&J separates from its orthopedics business, it's laying off 56 employees in New Jersey
- ASCO preview: With expectations jacked up, Akeso's ivonescimab to face scrutiny in high-stakes plenary
- An insider’s look at LillyDirect
- GLP-1 manufacturer CordenPharma strikes deal for peptide CDMO, lining up new production sites in US and China
- Weight-Loss Program Helps Women Battling Breast Cancer
- Younger U.S. Women of Color Face Rising Breast Cancer Deaths
- High Fitness Doesn’t Raise A-fib Risk In Young Men, Study Finds
- Cheaper, Alternative Health Plans Are Having A Moment, But Critics Urge Caution
- Ultrafine Wildfire Smoke Particles May Pose Serious Health Risks
- Montana Hurries To Adopt Trump’s Medicaid Work Rules Amid Budget Woes
- Readers Address Drugged Driving, Suicide Prevention, Worker Shortages
- Nurse Convicted in Patient’s Death Turns Fatal Drug Error Into a Cautionary Tale
- Amid policy and pricing headwinds, US healthcare and life sci faces 'vast field of opportunity': survey
- Amid policy and pricing headwinds, US healthcare and life sci faces 'vast field of opportunity': survey
- Biogen investigated by Italian regulator over multiple sclerosis ‘market abuse’ claims
- FDA delays ruling on AstraZeneca’s breast cancer drug after negative adcomm vote
- Eli Lilly wins argument over Noom’s GLP-1 dosing claims
- Remarks at the Stanford Rock Center for Corporate Governance
- Smart ring maker Oura files confidentially for IPO as consumer demand propels revenue growth
- Outlook moves toward potential US nod for thrice-snubbed eye drug with FDA appeal win
- JD Power: Cost pressures worsen member experience with commercial plans
- Trump Admin Bars Key U.S. Researchers From Global Virus Response Talk
- Listen to the Latest ‘KFF Health News Minute’
- As calls for COINS Act expansion grow, will new rules sweep up China biotech licensing?
- Everyone Has A Family Doc, But Can You Get An Appointment?
- Many U.S. College Students With Psychosis Are Not Receiving Treatment
- Antibiotics Won't Help Ease Asthma-Linked Wheezing in Kids
- Yoga Eases Insomnia And Anxiety In Cancer Survivors, Study Finds
- Dust Yields Clues to Viral Outbreaks, Study Finds
- 3 Medical Routines That Older People May Not Need
- Acting NIAID Chief Steps Down Amid Ebola, Hantavirus Concerns
- Sunscreen Confusion Puts More Americans At Risk For Melanoma
- 1 In 10 U.S. Surgeons Quit Practice, Study Warns Of Shortage
- Video Game Can Detect Depression In Minutes, Study Says
- Quitting Smoking Might Lower Your Dementia Risk
- Severe Asthma Often Comes With Other Serious Health Problems
- Efforts To Understand The Nation's Drugged Driving Problem Stall Under Trump
- RFK Jr. Fires Two Leaders Of Major U.S. Health Task Force
- Common Food Preservatives Linked to Major Heart Problems
- Migraine With Aura Linked To Middle-Age Stroke Risk
- Nicotine Vapes Triple Smokers' Odds Of Quitting Tobacco
- Fatty Liver Disease Increases Heart Attack Risk, Study Says
- Fixing Eligibility at the Point of Care: The Missing Link in Medical Device Reimbursement Integrity
- Fixing Eligibility at the Point of Care: The Missing Link in Medical Device Reimbursement Integrity
- The failure of the ‘usual suspects’ approach to life science recruitment
- The failure of the ‘usual suspects’ approach to life science recruitment
- Statement on Novel Exchange-Traded Funds (ETFs)
- Value, Focus, and the Future of MedTech: M&A and Divestitures are Rewriting the Strategic Playbook.
- Value, Focus, and the Future of MedTech: M&A and Divestitures are Rewriting the Strategic Playbook.

This NIH racialist program grant may or may not be associated with the MDHHS Advancing Healthy Births plan:
https://obgyn.msu.edu/research/the-miracle-center
MATERNAL HEALTH MULTILEVEL INTERVENTIONS FOR RACIAL EQUITY (MIRACLE) CENTER
Reducing disparities in pregnancy-related illness and death among African American, Hispanic, and rural populations in Michigan.
The Center will be rooted in a culturally informed research community with longstanding involvement from community, health, and policy partners. Critically important partners will also include Black and Hispanic Medicaid-eligible mothers, parents, and their families.
Cris Meghea, Jennifer E. Johnson, and Peggy Vander Meulen lead the Center (U54HD113291). Supporting the Department, College, and University commitment to advance women’s health and health equity, this U54 Maternal Health Research Center of Excellence was funded to address maternal morbidity and mortality disparities across Michigan. It is one of 10 Centers of Excellence nationwide that NIH is funding through their IMPROVE (Implementing a Maternal health and PRegnancy Outcomes Vision for Everyone) initiative. The NIH funding amount for the Center is close to $19 mil. over 7 years starting in 2023.
Birthing individuals and their families in 20 counties throughout Michigan will be impacted by the work of the Center, covering a population of more than 7 million individuals.
The Center’s groundbreaking work will be led by members of partnering communities and Michigan State University faculty. The work will reduce disparities by implementing and testing interventions to reduce maternal illness and death through three projects - each with novel designs covering the pregnancy through postpartum periods. These projects will all build off each other, address multiple levels needed to create meaningful change, and work across several health systems.
In addition to information on how well the projects are running, the Center will collect information on pregnancy-related death and a wide range of pregnancy-related illnesses. The Center will also have access to a linked Michigan Medicaid dataset. This connection will allow the Center to organize information across projects and other national Centers. The Center will use this information to find the main effects of each project, the combined effects across projects, and ways to sustain and scale-up the work.
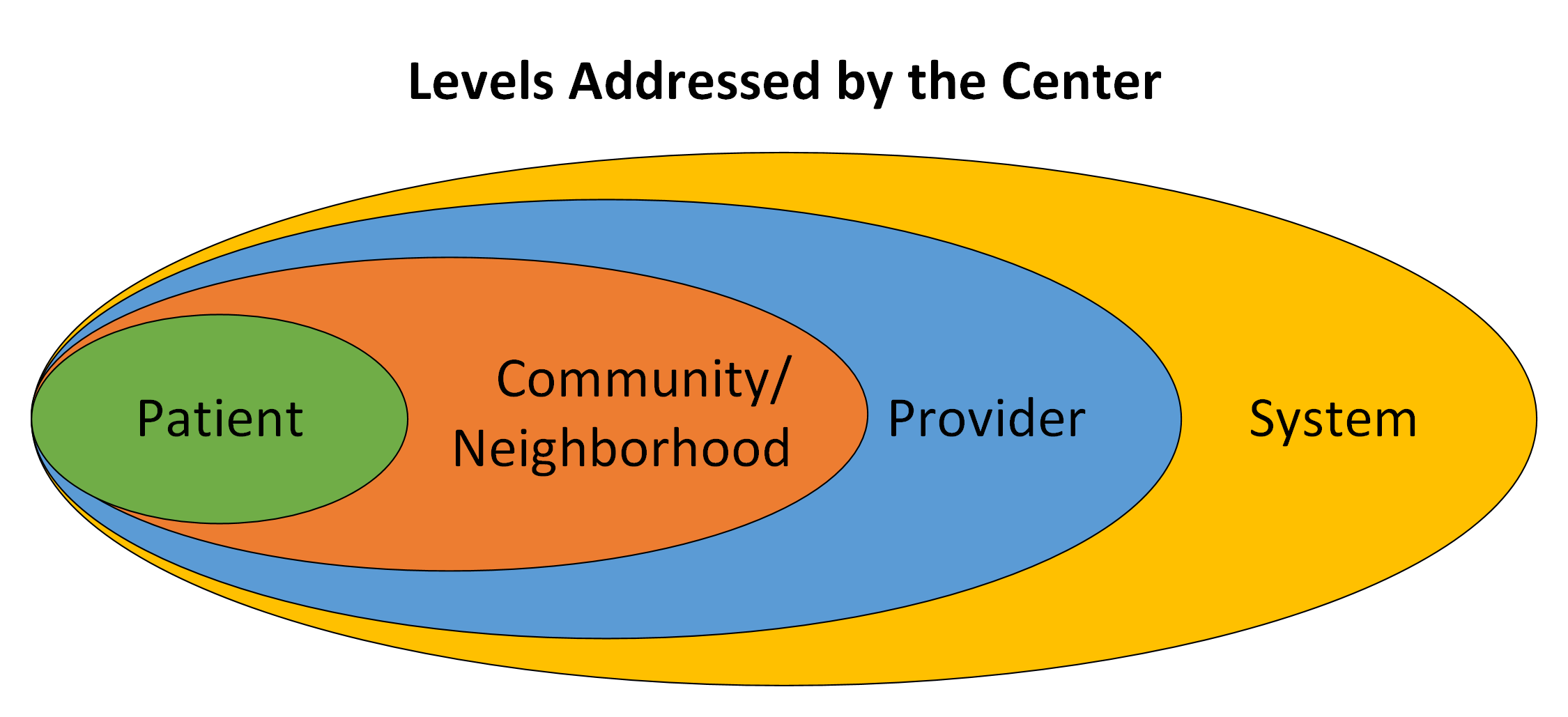
This Center will address the need for multilevel, community-centered, equity-focused interventions developed and tested with an emphasis on scalability and sustainment to address disparities in pregnancy-related illness and death.
Primary Investigators
Cris Meghea, PhD
He/Him
Associate Professor of Obstetrics, Gynecology, and Reproductive Biology
Director and Co-Founder of the Advancing Maternal Health Equity LabJennifer E. Johnson, PhD
She/Her
C.S. Mott Endowed Professor of Public Health
Professor of OBGYN
Professor of Psychiatry and Behavioral MedicinePeggy Vander Meulen, MSN, RN
She/Her
Program Director of Strong BeginningsCenter investigators include Steve Ondersma, Claire Margerison, LeeAnne Roman, Kent Key, Alla Sikorskii, Jim Dearing, Rick Leach, Hannah Bolder, and Xiao Yu from MSU; Kimberlydawn Wisdom and Jaye Clement from HFH; Peggy Vander Meulen and Celeste Sanchez-Lloyd from Corewell Health; E. Hill De Loney and Sharon Saddler from Flint Community Based Organization Partners (CBOP), Athena McKay from Flint Innovation Solutions, and Bob Sokol from Wayne State University. The Center and every core have both academic and community PIs.
Community and health partners in MI and nationally include the Flint Community Based Organization Partners (CBOP), Hurley Medical Center, Munson Healthcare, MyMichigan Health, MDHHS, MiCHWA - Michigan
Community Health Worker Alliance, AIM CCI - Alliance for Innovation on Maternal Health—Community Care Initiative, and others.
This Center will reduce pregnancy-related and pregnancy-associated maternal morbidity and mortality (PRAMM) disparities in African American, Hispanic, and rural populations through innovative and culturally relevant community-partnered effectiveness and implementation research. The Center tests multilevel, community-centered, equity-focused interventions for PRAMM disparities, with an emphasis on scalability and sustainment. It is also home to a community partnership consortium and training program.
Project 1: Multilevel community-centered intervention to reduce pregnancy related and associated morbidity and mortality (PRAMM) disparities in non-Hispanic Black and Hispanic Medicaid-insured individuals.
Investigators: Meghea, Slaughter-Acey, and Wisdom
This project is the first large-scale test of a home visiting program that integrates community health workers to focus on PRAMM disparities issues, including comorbid conditions. It will address patient-provider interactions from provider and patient perspectives.
Project 2: High reach, multi-level digital intervention for pregnancy-related and -associated morbidity and mortality (PRAMM) disparities.
Investigators: Ondersma, Margerison, and McKay
This project develops and tests the effectiveness of a technology-enabled approached to reducing PRAMM disparities among rural and African American populations.
Project 3: Scale-up implementation approaches to ending pregnancy-related and -associated morbidity and mortality (PRAMM) disparities.
Investigators: Johnson and Clement
This project will develop and evaluate the effectiveness and cost-effectiveness of a scale-up implementation approach for scaling equity-focused outpatient and community care safety bundles county-wide in 12 Michigan counties with a population of nearly 6 million people.
Community Partnership Consortium
Investigators: Key and Sanchez-Lloyd
This Consortium will create an action-oriented, inclusive, broad-based stakeholder group to act as full partners in increasing the relevant and reach of Center activities.
Training program addressing the multilevel factors that affect pregnancy-related and pregnancy-associated morbidity and mortality disparities
Investigators: Margerison, Meghea, and Saddler
The Center will engage and prepare early-stage investigators, especially those from backgrounds or identities currently underrepresented in the health sciences, to conduct research that address the biological, behavioral, environmental, and structural determinants of PRAMM disparities.
The NIH press release:
https://www.nichd.nih.gov/newsroom/news/081723-Maternal-Health-Research-Centers
Release: NIH establishes Maternal Health Research Centers of Excellence
Initiative to support research to reduce pregnancy-related complications and deaths and promote maternal health equity
Credit: NICHDThe National Institutes of Health has awarded $24 million in first-year funding to establish Maternal Health Research Centers of Excellence. Part of NIH’s Implementing a Maternal health and PRegnancy Outcomes Vision for Everyone (IMPROVE) initiative, the centers will develop and evaluate innovative approaches to reduce pregnancy-related complications and deaths and promote maternal health equity. The grants are expected to last seven years and total an estimated $168 million, pending the availability of funds.
Compared to other high-income countries, the United States has a high rate of maternal deaths, with more than 1,200 such deaths occurring in 2021, the most recent year for which data are available. Each year tens of thousands more Americans experience severe pregnancy-related complications, which can raise the risk of future health concerns, including high blood pressure, diabetes and mental health conditions. There are stark disparities in these maternal health outcomes by racial and ethnic group, age, education, socioeconomic status and geographic region.
“The magnitude and persistence of maternal health disparities in the United States underscore the need for research to identify evidence-based solutions to promote health equity and improve outcomes nationwide,” says Diana W. Bianchi, M.D., director of NIH’s Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD). “Through collaborations with community partners and others, the Maternal Health Research Centers of Excellence will generate critical scientific evidence to help guide clinical care and reduce health disparities during and after pregnancy.”
NICHD, the NIH Office of Research on Women’s Health and the National Institute of Nursing Research co-lead the IMPROVE initiative, with involvement from several other components at NIH.
The centers of excellence include 10 research centers, a data innovation and coordinating hub and an implementation science hub. Together, these institutions will work to design and implement research projects to address the biological, behavioral, environmental, sociocultural and structural factors that affect pregnancy-related complications and deaths. They will focus on populations that experience health disparities, including racial and ethnic minorities, socioeconomically disadvantaged populations, those living in underserved rural areas, sexual and gender minority populations and people with disabilities.
Research centers will partner with community collaborators, such as state and local public health agencies, community health centers and faith-based organizations. Additionally, the research centers will support training and professional development of maternal health researchers, including those from backgrounds underrepresented in the biomedical research workforce.
Funding for the centers was awarded after a competitive peer review process. The following institutions, listed alphabetically along with project name and contact principal investigator, will participate as research centers:
- Avera McKennan Hospital, Sioux Falls, South Dakota
Maternal American-Indian Rural Community Health (MARCH)
Principal investigator: Amy J. Elliott, Ph.D.- Columbia University, New York City
NY Community-Hospital-Academic Maternal Health Equity Partnerships (NY-CHAMP)
Principal investigator: Uma Reddy, M.D.- Jackson State University, Jackson, Mississippi
Delta Mississippi Center of Excellence in Maternal Health
Principal investigator: Mary D. Shaw, Ph.D.- Medical College of Wisconsin, Milwaukee
Addressing Key Social-Structural Risk Factors for Racial Disparities in Maternal Morbidity in Southeastern Wisconsin (ASCEND WI)
Principal investigator: Anna Palatnik, M.D.- Michigan State University, East Lansing
Maternal Health Multilevel Intervention/s for Racial Equity (MIRACLE) Center
Principal investigator: Cristian Ioan Meghea, Ph.D.- Morehouse School of Medicine, Atlanta, Georgia
Center to Advance Reproductive Justice and Behavioral Health among Black Pregnant/Postpartum Women and Birthing People (CORAL)
Principal investigator: Natalie Dolores Hernandez, Ph.D.- Stanford University, Stanford, California
Stanford PRIHSM: Preventing Inequities in Hemorrhage-related Severe Maternal Morbidity
Principal investigator: Yasser Y. El-Sayed, M.D.- Tulane University, New Orleans
Southern Center for Maternal Health Equity
Principal investigator: Emily Wheeler Harville, Ph.D.- University of Oklahoma Health Sciences Center, Oklahoma City
Center for Indigenous Resilience, Culture, and Maternal Health Equity
Principal investigator: Karina M. Shreffler, Ph.D.- University of Utah, Salt Lake City
ELEVATE Center: Reduction of Maternal Morbidity from Substance Use Disorder in Utah
Principal investigator: Torri D. Metz, M.D.Johns Hopkins University, Baltimore, will serve as the data innovation and coordinating hub. Led by principal investigator Andreea Creanga, M.D., Ph.D., this hub will support data collection, ensure high data quality and provide data science expertise. The University of Pennsylvania, Philadelphia, will serve as the implementation science hub. Under the direction of principal investigator Meghan Brooks Lane-Fall, M.D., this hub will help to promote the integration of research findings and evidence into public health, clinical practice and community settings.
About the Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD): NICHD leads research and training to understand human development, improve reproductive health, enhance the lives of children and adolescents, and optimize abilities for all. For more information, visit https://www.nichd.nih.gov .
About the National Institutes of Health (NIH): NIH, the nation's medical research agency, includes 27 Institutes and Centers and is a component of the U.S. Department of Health and Human Services. NIH is the primary federal agency conducting and supporting basic, clinical, and translational medical research, and is investigating the causes, treatments, and cures for both common and rare diseases. For more information about NIH and its programs, visit https://www.nih.gov .
A Detroit Free Press story on the MIRACLE Center with some explosive quotes:
Michigan gets $19M federal grant to tackle racial health disparities in pregnant, new moms
By Kristen Jordan Shamus - October 12, 2023Researchers at Michigan State University, Henry Ford Health and Corewell Health are launching a new, $19 million research center aimed at reducing disparities in pregnancy-associated deaths among Black, Hispanic, American Indian/Alaska Native women, and those who live in rural areas of the Lower Peninsula.
Called the Multilevel Interventions to Advance Maternal Health Equity Center, or the MIRACLE Center, it's one of 10 nationally to win funding from the National Institutes of Health to address racial health disparities in maternal mortality. It also is the first of its kind in Michigan.
"It is absolutely appalling to see the rates (of maternal mortality) that this country has experienced, given the wealth and the resources that we have," said Peggy Vander Meulen, director of Kent County’s Strong Beginnings, manager of community health programs at Corewell Health and a co-leader of the MIRACLE Center.
Researchers at Michigan State University, Henry Ford Health and Corewell Health are collaborating to launch a new, $19 million research center aimed at reducing disparities in pregnancy-associated deaths among Black, Hispanic, American Indian/Alaska Native women, and those who live in rural areas of the Lower Peninsula.
"What is the most upsetting is not only that maternal mortality overall has increased, but the rising disparities and inequities, particularly for Black and indigenous persons and also for Latino persons."
The underlying driver, she said, is "the systemic, institutionalized and structural racism that is been intentionally woven into the fabric of the society from the very beginning, and continues to intentionally or unintentionally result in inequities."
It affects everything from employment opportunities to access to safe and affordable housing, transportation and child care — and increases the risk that a woman will die during pregnancy and in the year after a baby is born, Vander Meulen said.
Black women 2.8 times more likely to die of pregnancy-related causes
In Michigan, the state Department of Health and Human Services reports that of the 80-90 maternal deaths that occur each year, 64% are preventable.
Black women in Michigan were 2.8 times more likely to die from pregnancy-related causes in 2015-19 than white women. The maternal mortality rate for Black women was 29.8 per 100,000 live births. For white women, it was 10.7 deaths per 100,000 live births, according to state data.
"The cause of all the disparities are racism, racism and racism," said Jennifer Johnson, C.S. Mott Endowed professor of public health in the MSU College of Human Medicine, and a co-leader of the MIRACLE Center.
"We're looking at two different kinds of disparities: One is the direct medical causes. Another is suicide, overdose, homicide. I think people are clear (in understanding) how the suicide, overdose, homicide deaths are responses to life stress. But more than half of the deaths occur after birth. ... If a mom is just trying to make ends meet, she may not go back for a two-week or a six-week checkup or she may be having headaches or she may be having shortness of breath. These other concerning symptoms and just sort of shake off or think, 'Oh, I don't have time for this' and then she dies."
Support for new mothers falls short
Exacerbating the problem is a lack of support for families, Vander Meulen said.
"People talk a great line about family values. However, we don't have ... mandatory parental leave or affordable child care," she said. "How do we expect parents and children to thrive? We have clients going back to work two weeks after delivery because they can't afford the time off. They can't afford to miss work at the minimum-wage jobs they're working just to keep food on the table."
Peggy Vander Meulen, director of Kent County’s Strong Beginnings and manager of community health programs at Corewell Health, is among the leaders of a new, $19 million project to study and reduce racial health disparities among pregnant and post-partum women in Michigan.
The rate of maternal mortality in Michigan more than doubled from 2018 to 2019 to a rate of 23.2 pregnancy-related maternal deaths per 100,000 live births. Official data on maternal mortality in Michigan for 2020, the first year of the coronavirus pandemic, won’t be released until early 2024, state health officials told the Free Press for a previous story.Access to health care also is a problem, both in rural parts of the state as well as urban centers, said Cristian Meghea, an associate professor of obstetrics, gynecology and reproductive biology in the MSU College of Human Medicine and co-leader of the MIRACLE Center.
"Having Medicaid insurance, that's great," Meghea said. "However, securing access to care and having an OB-GYN or even a general practitioner accepting new patients on Medicaid, that's a whole different problem. And a third problem is reaching that provider ... without having a car or without having reliable bus transportation. Or, being late and then getting your appointment canceled. These are all multiple hoops that that a lot of women have to go through."
Cristian Meghea, an associate professor of obstetrics, gynecology and reproductive biology in the Michigan State University College of Human Medicine and co-leader of the MIRACLE Center.
More:At least 60% of maternal deaths in Michigan are preventableAccess to care isn't enough. Women also need respect
Johnson added that even when people overcome all those barriers, they may face overt or implicit racism in the doctor's office.
"Once you get there, there's a respect issue. Am I being listened to? Am I being heard? Am I being respected when I voiced my concerns? Is my partner being respected when he joins me or when he is unable to join me?
Jennifer Johnson is a C.S. Mott Endowed professor of public health in the Michigan State University College of Human Medicine, and a co-leader of the MIRACLE Center.
"And so you have all these layers that contribute to mom saying, 'Well, yeah, I can find a provider. I have one, but when I go, I'm being so disrespected, I don't want to go. I'm willing to just wait it out until delivery and just show up to the emergency room.' And so that's another component of how do we make sure we're getting women not just access to care, but the proper and respected care that they deserve?"The center is launching three projects that begin immediately and will continue for seven years across 20 counties in the Lower Peninsula.
Project 1: Community health workers, visiting nurses and social workers will periodically visit the homes of pregnant and postpartum Black and Hispanic women in Kent, Wayne and Genesee counties to coordinate community and clinical care.
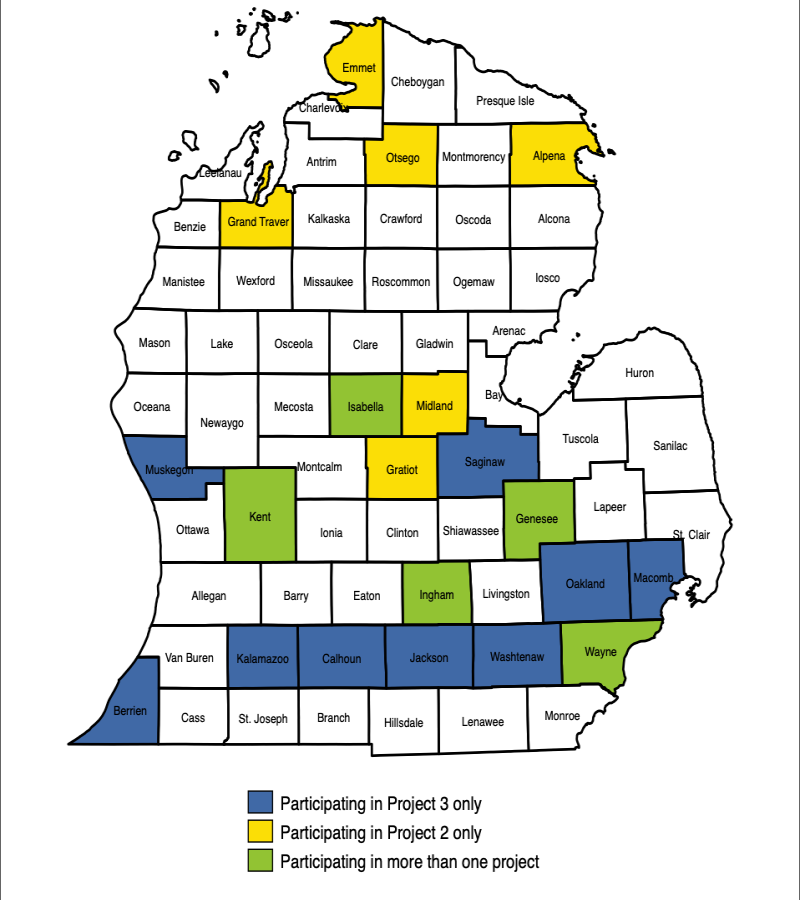
Project 2: Expands the use of a self-screening digital application that pregnant Black women and women living in rural areas can use to identify health warning signs. They can use it to live chat with community health workers who can connect them with services in 10 counties: Kent, Genesee, Ingham, Isabella, Emmet, Grand Traverse, Otsego, Alpena, Midland and Gratiot.
Project 3: Works to identify the best ways to improve equity in maternal care across 14 Michigan counties, focusing on improvement in the quality of care in both the medical setting and within the community. The counties involved are: Genesee, Kent, Wayne, Oakland, Ingham, Isabella, Macomb, Muskegon, Calhoun, Jackson, Saginaw, Kalamazoo, Berrien and Washtenaw.
"It is possible to improve the overall quality of obstetric care without changing disparities," Johnson said. "What Project 3 does is it looks at quality improvement efforts, targeting outpatient care and community care, and enhanced prenatal care because that's where most of the deaths occur. It looks at quality improvement approaches that directly target disparities.
"Despite some of the biases, white moms are actually more likely to die by overdose in pregnancy and postpartum than African American moms. But our African American moms are much more likely to die by homicide. As a matter of fact, for African-American women, the risk of dying by partner violence while pregnant increases eight fold.
"In general, if a woman dies, more than half the time it is by a current or former partner. Most of the deaths ... are suicide, overdose, homicide.
The MIRACLE Center will work through partnerships among university researchers, doctors, nurses and others at Henry Ford Health, Corewell Health, the Flint Community Based Organization Partners, Flint Odyssey House, Hurley Medical Center, Munson Healthcare, MyMichigan Health, and the Michigan Department of Health and Human Services.
Get MHF Insights
News and tips for your healthcare freedom.
We never spam you. One-step unsubscribe.