- Former clinic CEO pleads guilty to filing false tax returns
- Post Title
- North Carolina heart tower project enters CON race
- 45 ‘Best Companies for the Future’ in healthcare: WSJ
- How UC San Diego Health is making AI a core operating model
- Hartford Healthcare acquires cardiology group after antitrust settlement
- Arkansas system taps dual CEO, CFO
- Banner Health taps chief AI, data and infrastructure officer
- Just 5 Minutes Of Prayer Helps Reduce Pain and Anxiety, Study Finds
- 405 hospitals with the lowest CLABSI rates
- ‘Men don’t see themselves reflected in nursing’: How leaders can close the gap
- 5 resources on the operational fundamentals shaping healthcare in 2027
- Medtronic Advances Hugo Robotic Surgery Platform with Key FDA Filings and Product Approvals
- Medtronic Advances Hugo Robotic Surgery Platform with Key FDA Filings and Product Approvals
- Medtronic Posts Strongest Revenue Growth in a Decade, Driven by Cardiovascular and Surgical Businesses
- Medtronic Posts Strongest Revenue Growth in a Decade, Driven by Cardiovascular and Surgical Businesses
- Boston Scientific Plans Indiana Distribution Center, 300 New Jobs
- Boston Scientific Plans Indiana Distribution Center, 300 New Jobs
- Insurer-owned CAQH rebrands to DataSpring
- ADHD ‘Masking’ May Help People Blend In But Harms Mental Health
- Why Alcohol Makes You Crave Salty Snacks — And How Protein-Rich Foods Can Help Prevent Weight Gain
- Getting The RSV Shot While Pregnant Could Protect Your Baby After Birth
- Irregular Sleep Risks Preschool Kids' Brain Power
- Upcoming Billing Change Could Make Pregnancy Pricier
- By September, Nearly a Third of Americans Will Live in States With Legal Aid in Dying
- MAHA’s Treatments for Autism: Camel’s Milk, Stem Cell Injections — And Spelling Therapy
- Hikma earmarks $267M to expand pair of Ohio production sites, add 350 jobs
- Stepful banks $55M to scale AI-powered medical training to boost the workforce pipeline
- ADA: Amgen highlights Repatha perks, GLP-1 pitfalls in push to boost cardiometabolic pedigree
- Gounder Fills In Details Behind Ebola, GLP-1, and Trump Headlines
- The rise of the invisible patient experience
- Lifepoint among latest to file underpayment complaint against MultiPlan, insurers
- Untreated Cancer, Festering Infections: Immigrant Detainees Detail Medical Care Lapses
- Elation Health acquires Aster as it ramps up agentic AI for primary care
- Virginia dental practice suffers data breach affecting 5,200 individuals
- CRNAs could gain foothold in Medicare payment models
- Virginia oral surgery practice suffers data breach affecting 7,000 individuals
- 3 cases redrawing the lines of physician contracting
- ‘IDR is the exception, not the rule’: TeamHealth CMO on billing reality
- States ranked by mental health social workers per capita
- UnitedHealthcare cut CRNA pay 15% — are ASCs picking up the tab?
- Waco Cardiology’s research arm acquired in 3-city deal
- New York opens 60-bed OUD recovery center
- Kratom admissions jump 525% at California treatment center
- Buy, join or partner? Dentists’ advice for new grads
- The 10 states where ophthalmologists’ pay climbed the most
- Addiction Recovery Care founder indicted on fraud, money laundering charges
- Dengue Is No Longer Just A Travel Risk — What Google’s Mosquito Plan Could Mean For Your Summer
- Ohio targets behavioral health fraud with new oversight measures
- 12 state behavioral health policy updates
- California dental practice adds humanoid robot for front-desk help
- DentaQuest cybersecurity incident exposes 2.6 million accounts
- The 5 states with the most DSO action in May
- 5 highest-paying cities for dental assistants in 2026
- 5 highest-paying cities for hygienists in 2026
- 3 dental acquisitions in May
- 7 DSOs making headlines
- Brain Surgery For Pituitary Tumor Helps Illinois Mom Have Second Baby
- Essence Healthcare, Oura expand partnership to sleep apnea detection
- Takeda takes $2.5B legal charge after pay-for-delay verdict, swings to loss for '25
- Industry Voices—A healthcare experience that is as seamless as it is soulful
- Fullspan Health debuts Healthline AI companion to connect consumers to medical content and providers
- As pro-life pressure ramps up on Trump, FDA is investigating safety of abortion pill: WSJ
- As pro-life pressure ramps up on Trump, FDA is investigating safety of abortion pill: WSJ
- Popular Blood Pressure Meds, Dihydropyridine Calcium-Channel Blockers, Linked To Kidney Damage Risk In Type 2 Diabetes
- Too Much Sitting In Pregnancy Doubles Risk Of Complications
- Spinal Cord Stimulation May Restore Arm Strength After Stroke
- Behind the headlines of ASCO 2026
- RFK Jr. Seeks To Peek At Americans' Medical Records For Clues On Autism And Vaccines
- Two-Pill Combo, Inqovi and Venclexta, Offers Hospital-Free Leukemia Treatment Option For Older Adults With AML
- Millions of Kids Could Lose Insurance as GOP Healthcare Cuts Start To Bite
- ‘We Live With Fear’: In Congo, Doctors Face Ebola With Little Protection
- Upcoming Billing Change Could Make Pregnancy Pricier
- WellSpan Health strikes strategic partnership with Philips to deploy, co-develop new healthcare tech
- Oregon overhauls 30-year behavioral health agreement model: 3 things to know
- 6 states regulating AI in mental health
- RWJBarnabas Health sets 15K target for naloxone kit program
- 4 charged in $30M behavioral health fraud case
- At first public hearing for FDA’s CNPV program, industry support meets ‘deep concern’ from experts
- “Harmonization: We’ll Have Lots to Talk About”
- Remarks at the Investor Advisory Committee Meeting
- A Quarter for your Thoughts: Remarks at the Meeting of the SEC Investor Advisory Committee
- Weekly Rundown: Trump signs AI executive order; Health Catalyst to sell Vitalware for $147M
- Small businesses feel the squeeze as healthcare costs rise: Morgan Health
- Poll Finds Broad Support For Stricter Regulations On Ultra-Processed Foods
- It's unanimous: SCOTUS agrees with Hikma in 'skinny label' case vs. Amarin
- Remarks at the Investor Advisory Committee Meeting
- Fierce Pharma Asia—China's biotech rise; ASCO highlights; Lilly pipeline deals
- Nearly 1 in 5 Young People Turn to AI Chatbots for Mental Health Advice
- Ixlayer rolls out digital acute pain management platform in collaboration with Vertex Pharmaceuticals
- Georgetown study: 2M children have dropped out of Medicaid, CHIP since January 2025
- ScionHealth sends 8 community hospitals to Lifepoint Health
- ADC Therapeutics' shares plummet after patient deaths in trial of Zynlonta
- As China biotech crackdown calls reverberate in Washington, the pushback gets louder, too
- Older LGBTQ+ Adults Fear Less Support As They Age, Poll Shows
- Night Owls Are More Prone To Anxiety, Loneliness
- Home-Delivered Medical Meals Reduce ER Visits, Save Money
- Axsome fends off generic competition to narcolepsy med Sunosi until 2040
- Menopause Hormone Therapy Use Drops Sharply Across United States
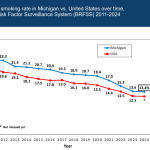
- Michigan Found A Way To Reduce School Vaccine Waivers — Until It Backfired
- Listen to the Latest ‘KFF Health News Minute’
- RFK Jr. Seeks To Peek at Americans’ Medical Records for Clues on Autism and Vaccines
- Louisiana’s Reporting Law Chills Immigrant Medicaid Applications
- Thyme Care expands cancer survivorship program to provide longitudinal support
- Medline earns FDA warning letter ire for repeated toxic bacteria problems
- 8 Requirements for AI Medical Interpreting: 2026 Survey Results
- Commonwealth Fund: 21% of adults experienced a coverage denial in the past year
- Healthcare Dealmakers—WakeMed to join Atrium Health, Qualtrics closes $6.8B Press Ganey deal and more
- Millions on Medicaid May Soon Have To Prove They’re Working To Keep Coverage
- Anomaly Insights launches AI solution for managed care executives
- Lilly, Boehringer to slash at least $1B each from planned investments in Germany
- Presbyterian Healthcare Services to discontinue MA plans in 2027, cut 150 jobs
- Just 90 Minutes Of Strength Training A Week Linked To Longer Life
- Amid Miplyffa launch, Zevra CEO aims to foster EU-style Niemann-Pick market in US
- Chemo-Free Drug, Tecvayli, Shows Major Survival, Remission Gains In Relapsed Multiple Myeloma
- Urine Test Can Detect Autism, Study Says
- High-Puff Vapes Become More Toxic Over Time, Study Says
- With Cencora pact, Gilead looks to grow CAR-T treatment center network
- Coffee, racetracks, beaches and more coffee—inside the ASCO 2026 exhibit floor
- GLP-1 Drugs Like Ozempic May Lower Breast Cancer Risk By About 30%
- Telehealth Booms As Demand For GLP-1s Surges and Questions Mount About Safety, Oversight
- A patient-first shift in disease language and communication
- FDA issues untitled letter after finding ‘eye-catching graphics’ in promotional emails
- Neurotech launches new YouTube channel to spotlight patients’ stories for rare eye disorder
- As Akeso takes center stage at ASCO, China biotech industry cements its coming of age
- Base Case: Remarks at the IC3 Blockchain Camp
- Department of Labor's proposed foreign worker wage increases are more tough news for healthcare staffing
- Trump Signs Order Calling For Fewer Childhood Vaccines
- Ascension closes its $3.9B AmSurg purchase following FTC's all-clear
- Simple Blood Test May Help Detect And Stage Alzheimer's Disease
- Marilyn Monroe and Amy Schumer profiled in endometriosis awareness push
- Smartphone App Helps Those With Advanced Cancer Maintain Quality Of Life
- Asthma Drug, Tezspire, Cuts Need For Steroid Pills While Keeping Attacks In Check
- Childhood Flu Shots Prevent Millions of Cases, Study Finds
- TikTok Videos Fuel Illicit Vaping Culture Among Underage Youth
- Amid Ebola, Hantavirus Outbreaks, Democrats Decry Trump's Health Cuts
- Commission Statement on the Passing of Former General Counsel David Becker
- Your Surprise Medical Bill May Be Gone — But Your Premiums Could Still Spike
- Short-Term Fasting Could Boost Chemo Response in Ovarian Cancer, Study Suggests
- MedTech In Focus: AI impact in healthcare
- MedTech In Focus: AI impact in healthcare
- If Your AI Can’t Explain Itself, Can FDA Authorize It?
- If Your AI Can’t Explain Itself, Can FDA Authorize It?
- Workout Habits May Protect Against Inherited Heart Problems
- Childhood Lying Is Normal and Rarely Signals Behavioral Concerns, Study Says
- Perfectionism Among College Students Reaches Record High, Fueling Anxiety
- After Her Bout of Amnesia, A $59,000 Billing Dispute Wouldn't Go Away
- Rising Stars: WPP’s Meghan O’Hora on the ‘complex puzzle’ of oncology drug marketing
- Climate Change: Statement on Proposed Rescission of Climate-Related Disclosure Rules
- Statement of Commissioner Mark T. Uyeda on the Rescission of Climate-Related Disclosure Rules
Michigan healthcare freedom community forum
We have a physician shortage. (Or at least, a shortage of physicians who want to work in our broken system. Which is to say, not enough physicians to enter all the data our central planners want entered. About us.)
If you were to reform MD education by committee - oh wait.
They already published it.
Here you go, from the Accreditation Council for Graduate Medical Education (ACGME).
Summary of Proposed Changes to ACGME Common Program Requirements Section VI
In developing the revised standards, the Common Program Requirements Phase 1 Task Force considered all available information, including relevant literature, written comments received from the graduate medical education community and the public, and testimony provided during the ACGME Congress on the Resident Learning and Working Environment. Deliberations of the Task Force were guided by the need to develop standards that: (1) emphasize that graduate medical education programs are designed to provide professional education; (2) are based on the best available evidence; and (3) support the philosophy outlined in the preamble to the revised requirements.
The revised requirements are intended to promote patient safety, resident well-being, and inter-professional team-based care by providing greater flexibility within an established framework, allowing programs and residents more discretion to structure clinical education in a way that best supports the principles of professional development. With this increased flexibility comes the responsibility for programs and residents to adhere to the 80-hour maximum weekly limit, and to utilize flexibility in a manner that optimizes patient safety, and resident well-being and education. In addition, the requirements eliminate the documentation requirement for residents to justify clinical and educational work hour variations.
Clinical and educational work hours represent only one part of the larger issue of conditions of the learning and working environment, and Section VI has now been expanded to include greater attention to patient safety and resident and faculty member well-being. The requirements are intended to support programs and residents as they strive for excellence, while also ensuring ethical, humanistic training. Ensuring that flexibility is used in an appropriate manner is a shared responsibility of the program and residents. With this flexibility comes a responsibility for residents and faculty members to recognize the need to hand off care of a patient to another provider when a resident is too fatigued to safely provide care and for programs to ensure that residents remain within the 80-hour maximum weekly limit.
Summary of Changes
VI.A.Patient Safety, Supervision, and Accountibility
These new and expanded requirements have been added in recognition of the need to make explicit that resident education must occur in an environment designed to emphasize a culture of safety and quality improvement, with appropriate levels of supervision and accountability. This increased emphasis on patient safety and quality improvement is expected to improve resident education and patient safety. It is necessary that residents and faculty members consistently work in a well-coordinated manner with other health care professionals to achieve institutional patient safety goals, such as consistent reporting and disclosure of patient safety and adverse events. It is essential that residents learn both to identify the causes of patient safety events, and to institute sustainable systems-based changes to ameliorate patient safety vulnerabilities. This includes receiving data on quality metrics and benchmarks related to their patient populations. Finally, although the attending physician is ultimately responsible for the care of the patient, every physician shares in the responsibility and accountability for his or her efforts in the provision of care. Supervision in the setting of graduate medical education provides safe and effective care to patients; ensures each resident’s development in the skills, knowledge, and attitudes required to enter unsupervised practice; and establishes a foundation for continued professional growth. The revisions to the requirements regarding supervision of residents were made to emphasize the expectation that an individual resident’s level of training and the patient complexity and acuity must factor into decisions regarding the level of supervision provided to that resident, ensuring that the level of supervision is appropriate for each patient.
VI.B. Professionalism
This section describes professionalism in the broad context of what it means to be a physician, including the ultimate responsibility of provision of comprehensive care to the patient. These requirements make explicit that the program director and Sponsoring Institution must ensure a culture of professionalism that supports patient safety and personal responsibility, and that residents and faculty members must demonstrate an understanding an acceptance of their personal role in support of their patients’ safety, including accurate reporting of work hours, patient outcomes, and clinical experience data. Requirements in this section highlight the critical importance of awareness and accountability for fitness for duty, as well as the responsibility of all residents and faculty members to display responsiveness to patient needs that supersedes self-interest. This includes the recognition that under certain circumstances, the best interests of the patient may be served by transitioning care to another qualified and rested provider.
VI.C. Well-Being
The addition of expanded and more specific requirements regarding resident and faculty well-being emphasize the need for programs and institutions to prioritize well-being and recognize that physicians are at increased risk for burnout and depression. Programs and Sponsoring Institutions have the same responsibility to address well-being as they do to ensure other aspects of resident competence. Further, self-care is also an important aspect of professionalism, and a skill that must be learned and nurtured in the context of other aspects of graduate medical education. Promotion of well-being, ensuring protected time with patients, and minimization of non-physician obligations are expected to improve both resident education and quality of patient care. Key components of the requirements of programs and institutions in this area include:
- Helping residents find meaning in work: protected time with patients; minimizing non-physician obligations; administrative support; progressive autonomy and flexibility; enhancement of professional relationships
- Attention to scheduling, work intensity, and work compression
- Evaluating the safety of residents and faculty members in the learning and working environment
- Establishing policies and programs supporting optimal resident and faculty member well-being, including the opportunity to attend appointments for personal care, even during working hours
- Attention to and education in resident and faculty member burnout, depression, and substance abuse in themselves and others; provision of services and resources for care, and tools to identify symptoms and report them; and availability and access to confidential, affordable mental health counseling and treatment, including access to urgent and emergent care 24 hours a day, seven days a week.
- Establishing policies and procedures ensuring continuity of patient care in support of patient and physician safety when residents and faculty members are unable to work, including but not limited to circumstances related to fatigue, illness, and family emergencies.Click for more information about the ACGME’s efforts related to Physician Well-Being
VI.D. Fatigue Mitigation
These requirements specify program responsibility related to education of faculty members and residents in recognizing signs of fatigue to ensure continuity of patient care and the provision of adequate sleep facilities and safe transportation options for program residents.
VI.E. Clinical Responsibilities, Teamwork, and Transitions of Care
These requirements define the appropriate level of clinical responsibilities based on resident training level and patient condition, and specify the need for provision of opportunities for residents to work in interprofessional teams appropriate to delivery of care in the specialty or subspecialty and larger health system. Requirements regarding optimization of care transitions in support of continuity of care and patient safety are included here. The requirements make explicit the responsibility of programs and Sponsoring Institutions to ensure and monitor effective, structured hand-over processes, and to ensuring that residents are competent in communications related to hand-offs.
VI.F. Clinical Experience and Education (formerly Duty Hours)
Programs and Sponsoring Institutions must design an effective program structure that provides work-life balance, enabling residents to gain requisite educational and clinical experience as well as reasonable opportunities for rest and personal activities. These requirements encompass the baseline priority for institutions and programs to provide a consistent opportunity for residents to experience an interdisciplinary team-based approach to patient care, safety, physician well-being, and education. Based on thorough review of the best available, current evidence, the cornerstone of these requirements, unchanged since the 2003 revision of the Common Program Requirements, remains the 80-hour weekly limit, one day off in seven, and in-house call no more often than every three days, averaged over four weeks. Programs are responsible for ensuring that residents are provided with manageable workloads that can be accomplished during scheduled work hours. This includes that residents have appropriate support from their clinical teams, and that they are not overburdened with clerical work and/or other non-physician responsibilities.
The terms “clinical experience and education,” “clinical and educational work,” and “work hours” replace the terms “duty hours,” “duty periods,” and “duty” in the proposed revision. This change was made to emphasize that residents’ responsibility to the safe care of their patients supersedes any duty to the clock or schedule.
Changes made in this section include:
Clinical work done from home must be counted toward the 80-hour weekly maximum.
Clinical work periods for all residents must not exceed 24 hours of continuous scheduled clinical assignments.
- This change is expected to improve resident education by permitting PGY-1 residents to more fully participate as members of the health care team, with appropriate supervision.Clinical work hour exceptions may be granted by the Review Committee to support specialty-specific rotations approved by the institution, for up to a maximum of 88 hours based on sound educational rationale.
Residents who have appropriately handed off patients following the conclusion of scheduled work periods have the flexibility to voluntarily remain at work in unusual circumstances, if, in their judgment, those circumstances benefit patient care or education. Such additional time must be counted toward the 80-hour limit.
All residents must have at least 14 hours free of clinical work after 24 hours of clinical assignments. Physicians have a responsibility to return to work rested, and thus are expected to use time away from work to get adequate rest. In support of this goal, residents are encouraged to prioritize sleep over other discretionary activities. Other requirements regarding time off between work periods have been modified to support resident education and patient safety by permitting programs increased flexibility to develop schedules that work best at the local level.
I wonder: will they make residents wear Fit-Bits to monitor their work load? Maybe the monitors can be programmed, like trucker logs, so their brains turn off when it's break time.
Get MHF Insights
News and tips for your healthcare freedom.
We never spam you. One-step unsubscribe.