- Dental implant provider lands growth investment
- Specialty1 Partners appoints VP of business development
- ‘Much needed clarity and a path to restore trust’: Fairview, U of Minnesota, M Physicians close in on new 10-year deal
- Maryland dental practice acquires 2nd office
- Physicians are not ‘providers’: AMA
- Stanford’s AI discharge summary tool cuts physician burnout
- Optum to cut 92 jobs in California
- R1 RCM names former Humana executive CIO
- 2 Oregon practices merge, creating one of state’s largest physician-owned groups
- 3 states take aim at private equity in healthcare
- UPMC lays off 200 workers, cuts 300 positions
- Google develops passive heart rate monitoring via smartphone camera
- Why AdventHealth thinks it can sell an internal insurance model to employers
- AHA: Hospitals lean on technology to make healthcare more affordable
- How Oceans Healthcare is scaling behavioral care — starting with the ER
- South Dakota health system names 2 executives
- 5 ASC leaders to know
- GLP-1 drugs tied to 75% lower substance use disorder odds: 4 notes
- When physician groups hit the wall: 3 turnaround stories
- 7 updates from Park Dental Partners since its IPO
- How general dentist pay compares to 25 healthcare roles
- 14 state behavioral health policy updates
- Who’s snatching up DSOs?
- The missed colonoscopy problem ASCs can no longer afford to ignore
- DEA finalizes OUD treatment rule: What it means for behavioral healthcare
- How Much Alcohol Is Actually Safe? A New Study Challenges Old Advice
- HCA Surgery Ventures names supply chain CEO
- 15 neurosurgeons to know
- CRNA pay is up 59% since 2019: 5 reasons why
- GLP-1s tied to lower risk of multiple cancers
- University of Pittsburgh dental school to open 3rd training center
- Colorado ‘screened out’ 92% of youth center abuse hotline calls: 5 things to know
- ASCs’ hidden efficiency drain
- Dental College of Georgia dean dies
- SF General, UCSF fined after social worker’s fatal stabbing
- Penn Medicine ED program boosts naltrexone prescriptions 15-fold
- Hundreds of hospitals warned over price transparency failings, AP reports
- Air Pollution Might Contribute To Clogged Arteries, Heart Disease Risk
- New Study Suggests No Major Adverse Outcomes With Early GLP-1 Exposure During Pregnancy
- Cleveland Clinic agrees to 'decades-long' halt on gender-affirming care for minors in DOJ settlement
- WuXi AppTec lands on Pentagon blacklist, facing Biosecure ban
- Merck, Gilead score in effort to develop the first weekly HIV pill
- As Gilead's Trodelvy stumbles in first-line lung cancer, all eyes turn to Merck, AZ and Daiichi rivals
- Clinicians report AI use expands patient capacity, boosts efficiency: Philips survey
- Feeding Babies Eggs Sooner May Cut Allergy Risk, Study Suggests
- At A Tennessee Hospital, Nurse Stole Fentanyl And AI Missed It, State Records Say
- Infections A ‘Major Health Hazard’ For People With Diabetes, Large Study Warns
- MAHA's Treatments For Autism: Camel's Milk, Stem Cell Injections — And Spelling Therapy
- Trivia Nights, Valentine’s Cards: Overlooked Social Connections Can Prevent Suicide
- Could Your Kid Benefit From Counseling? Experts Offer 3 Questions To Help You Decide
- AstraZeneca reprimanded over LinkedIn likes once again
- 29 behavioral health executive moves to know
- 3 states where dental hygienist pay dropped
- 5 states where dental assistant pay dropped
- ‘No disruptions’: Elevance study backs take-home methadone
- Dartmouth Health targets treatment gap for pregnant patients with SUD
- From affordability to engagement, these are the topics to watch at AHIP 2026
- Accrediting bodies, more medical schools commit to RFK Jr.'s nutrition education pledge
- Children's Well-Being Plummets Across 29 States, Report Finds
- Senate HELP committee chairman seeks info on NYC Health + Hospital data breach
- ADA: Lilly posts oral semaglutide-topping data as Foundayo speeds toward 2nd potential nod in diabetes
- With ADA in the books, analyst says Lilly is ‘widening its lead’ in the obesity race
- CVS launched an AI Learning Academy for its workforce. Here's why
- Just 5 Minutes Of Prayer Helps Reduce Pain and Anxiety, Study Finds
- Sophia Genetics, Memorial Sloan Kettering sign strategic collab for AI-powered precision oncology hub
- ‘Law & Order’ star Mariska Hargitay teams up with BMS to investigate multiple myeloma research in awareness campaign
- Medtronic Advances Hugo Robotic Surgery Platform with Key FDA Filings and Product Approvals
- Medtronic Posts Strongest Revenue Growth in a Decade, Driven by Cardiovascular and Surgical Businesses
- ADA: Novo's Wegovy pill reaches new GLP-1 patients with impressive 3M prescription milestone
- Boston Scientific Plans Indiana Distribution Center, 300 New Jobs
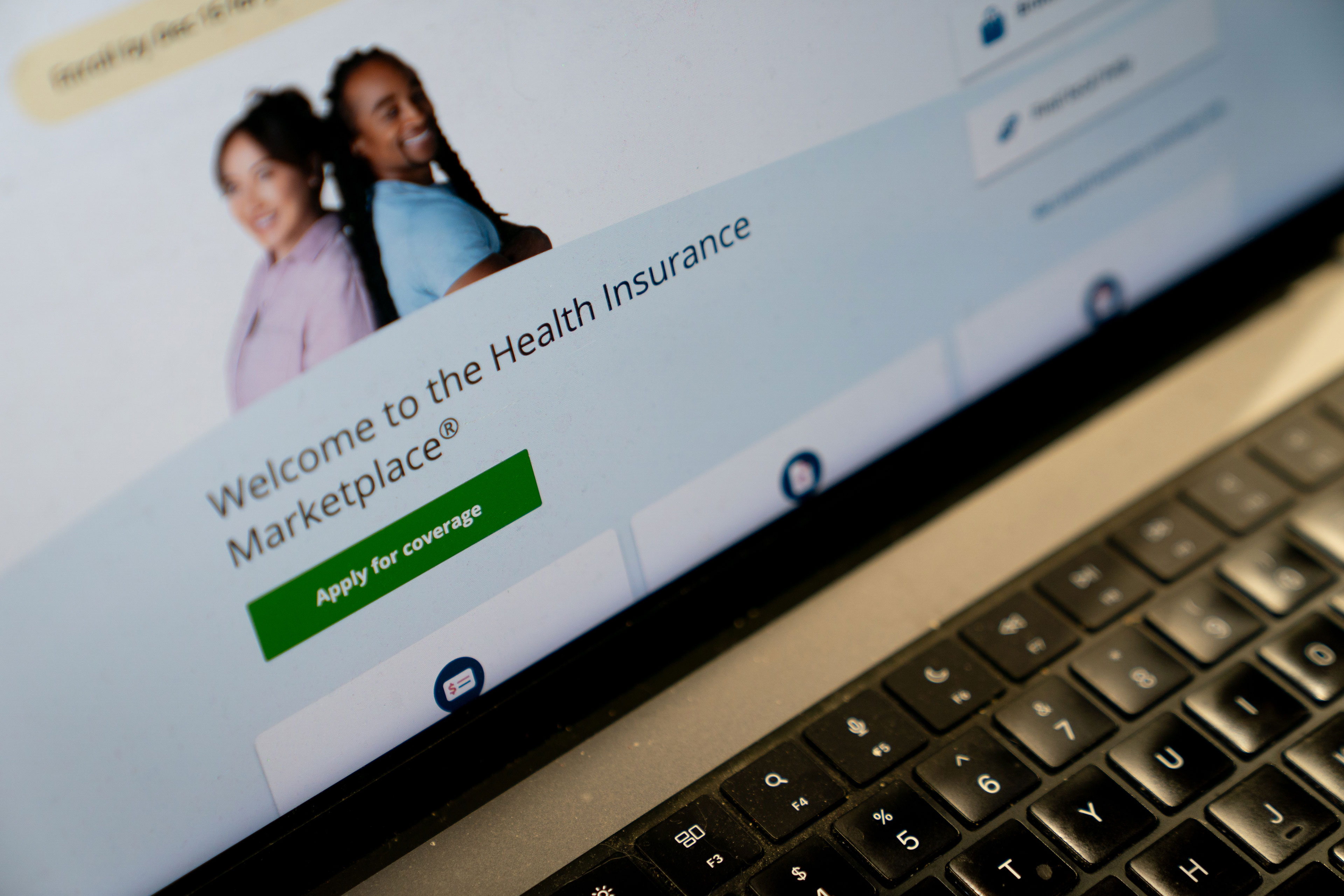
- Cities sue Trump administration to block final ACA rule
- Irregular Sleep Risks Preschool Kids' Brain Power
- Why Alcohol Makes You Crave Salty Snacks — And How Protein-Rich Foods Can Help Prevent Weight Gain
- ADHD ‘Masking’ May Help People Blend In But Harms Mental Health
- Getting The RSV Shot, Abrysvo, While Pregnant Could Protect Your Baby After Birth
- Pfizer scores FDA pediatric expansion for hemophilia treatment Hympavzi
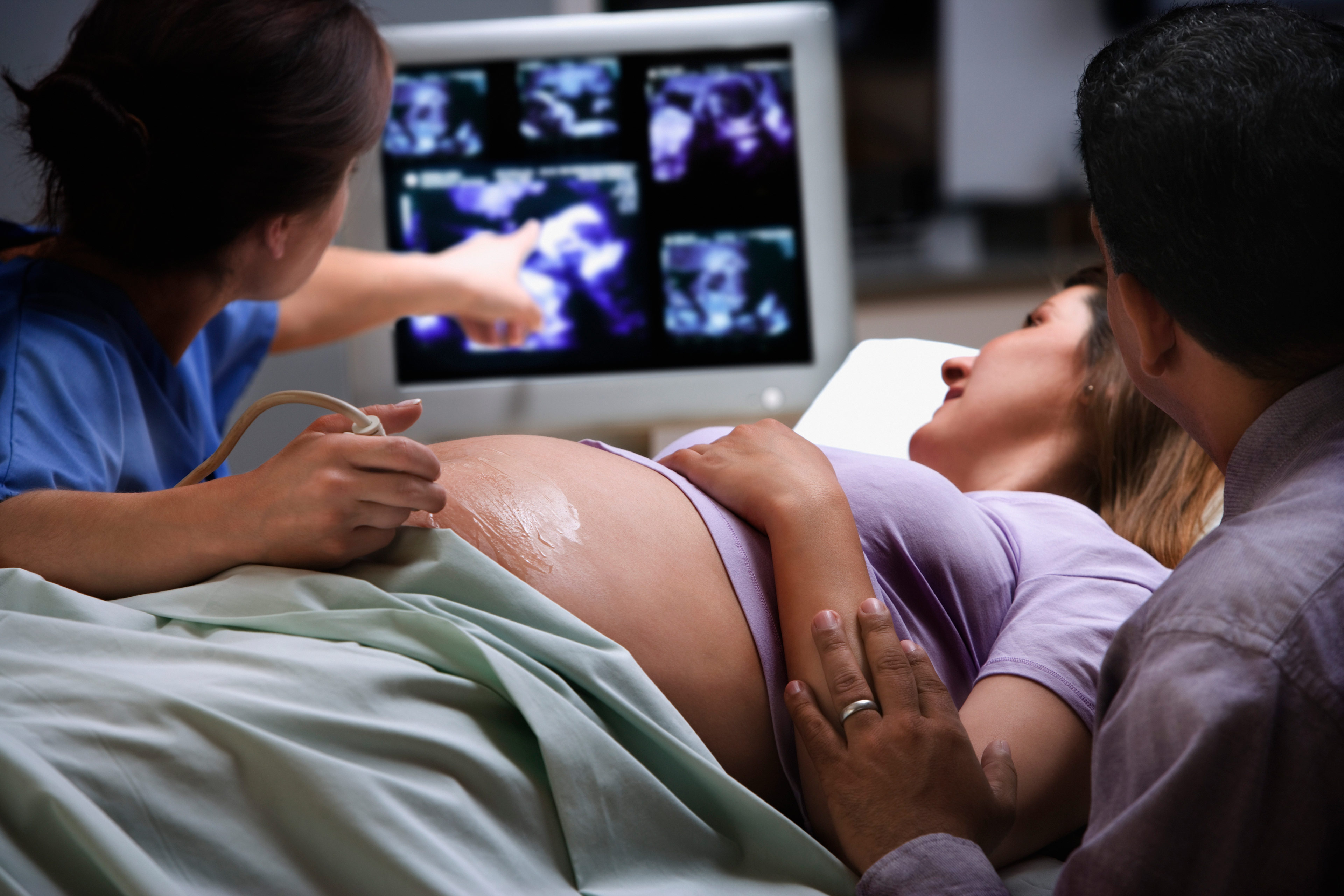
- Upcoming Billing Change Could Make Pregnancy Pricier
- MAHA’s Treatments for Autism: Camel’s Milk, Stem Cell Injections — And Spelling Therapy
- By September, Nearly a Third of Americans Will Live in States With Legal Aid in Dying
- Hikma earmarks $267M to expand pair of Ohio production sites, add 350 jobs
- Stepful banks $55M to scale AI-powered medical training to boost the workforce pipeline
- ADA: Amgen highlights Repatha perks, GLP-1 pitfalls in push to boost cardiometabolic pedigree
- Gounder Fills In Details Behind Ebola, GLP-1, and Trump Headlines
- Untreated Cancer, Festering Infections: Immigrant Detainees Detail Medical Care Lapses
- Elation Health acquires Aster as it ramps up agentic AI for primary care
- Dengue Is No Longer Just A Travel Risk — What Google’s Mosquito Plan Could Mean For Your Summer
- Brain Surgery For Pituitary Tumor Helps Illinois Mom Have Second Baby
- Essence Healthcare, Oura expand partnership to sleep apnea detection
- Takeda takes $2.5B legal charge after pay-for-delay verdict, swings to loss for '25
- Industry Voices—A healthcare experience that is as seamless as it is soulful
- Fullspan Health debuts Healthline AI companion to connect consumers to medical content and providers
- As pro-life pressure ramps up on Trump, FDA is investigating safety of abortion pill: WSJ
- As pro-life pressure ramps up on Trump, FDA is investigating safety of abortion pill: WSJ
- Popular Blood Pressure Meds, Dihydropyridine Calcium-Channel Blockers, Linked To Kidney Damage Risk In Type 2 Diabetes
- Too Much Sitting In Pregnancy Doubles Risk Of Complications
- Spinal Cord Stimulation May Restore Arm Strength After Stroke
- Behind the headlines of ASCO 2026
- RFK Jr. Seeks To Peek At Americans' Medical Records For Clues On Autism And Vaccines
- Two-Pill Combo, Inqovi and Venclexta, Offers Hospital-Free Leukemia Treatment Option For Older Adults With AML
- Millions of Kids Could Lose Insurance as GOP Healthcare Cuts Start To Bite
- Upcoming Billing Change Could Make Pregnancy Pricier
- ‘We Live With Fear’: In Congo, Doctors Face Ebola With Little Protection
- WellSpan Health strikes strategic partnership with Philips to deploy, co-develop new healthcare tech
- At first public hearing for FDA’s CNPV program, industry support meets ‘deep concern’ from experts
- “Harmonization: We’ll Have Lots to Talk About”
- Remarks at the Investor Advisory Committee Meeting
- A Quarter for your Thoughts: Remarks at the Meeting of the SEC Investor Advisory Committee
- Weekly Rundown: Trump signs AI executive order; Health Catalyst to sell Vitalware for $147M
- Small businesses feel the squeeze as healthcare costs rise: Morgan Health
- Poll Finds Broad Support For Stricter Regulations On Ultra-Processed Foods
- It's unanimous: SCOTUS agrees with Hikma in 'skinny label' case vs. Amarin
- Remarks at the Investor Advisory Committee Meeting
- Fierce Pharma Asia—China's biotech rise; ASCO highlights; Lilly pipeline deals
- Nearly 1 in 5 Young People Turn to AI Chatbots for Mental Health Advice
- Ixlayer rolls out digital acute pain management platform in collaboration with Vertex Pharmaceuticals
- Ixlayer rolls out digital acute pain management platform in collaboration with Vertex Pharmaceuticals
- ADC Therapeutics' shares plummet after patient deaths in trial of Zynlonta
- As China biotech crackdown calls reverberate in Washington, the pushback gets louder, too
- Older LGBTQ+ Adults Fear Less Support As They Age, Poll Shows
- Night Owls Are More Prone To Anxiety, Loneliness
- Home-Delivered Medical Meals Reduce ER Visits, Save Money
- Axsome fends off generic competition to narcolepsy med Sunosi until 2040
- Menopause Hormone Therapy Use Drops Sharply Across United States
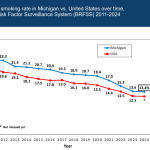
- Michigan Found A Way To Reduce School Vaccine Waivers — Until It Backfired
- Listen to the Latest ‘KFF Health News Minute’
- Medline earns FDA warning letter ire for repeated toxic bacteria problems
- 8 Requirements for AI Medical Interpreting: 2026 Survey Results
- Healthcare Dealmakers—WakeMed to join Atrium Health, Qualtrics closes $6.8B Press Ganey deal and more
- Millions on Medicaid May Soon Have To Prove They’re Working To Keep Coverage
- Just 90 Minutes Of Strength Training A Week Linked To Longer Life
- Chemo-Free Drug, Tecvayli, Shows Major Survival, Remission Gains In Relapsed Multiple Myeloma
- Urine Test Can Detect Autism, Study Says
- High-Puff Vapes Become More Toxic Over Time, Study Says
- GLP-1 Drugs Like Ozempic May Lower Breast Cancer Risk By About 30%
- Telehealth Booms As Demand For GLP-1s Surges and Questions Mount About Safety, Oversight
- Base Case: Remarks at the IC3 Blockchain Camp
- Trump Signs Order Calling For Fewer Childhood Vaccines
- Simple Blood Test May Help Detect And Stage Alzheimer's Disease
- Smartphone App Helps Those With Advanced Cancer Maintain Quality Of Life
- Asthma Drug, Tezspire, Cuts Need For Steroid Pills While Keeping Attacks In Check
- Childhood Flu Shots Prevent Millions of Cases, Study Finds
- Commission Statement on the Passing of Former General Counsel David Becker
- MedTech In Focus: AI impact in healthcare
- If Your AI Can’t Explain Itself, Can FDA Authorize It?
- Climate Change: Statement on Proposed Rescission of Climate-Related Disclosure Rules
- Statement of Commissioner Mark T. Uyeda on the Rescission of Climate-Related Disclosure Rules
- Keynote Remarks at the 2026 Reagan National Economic Forum
- Statement on Proposing Release for Rescission of Climate-Related Disclosure Rules
- Privacy and PetShops: Remarks at the Regulatory PETshop Series: Cryptographic Technologies and Financial Services Regulation
- CAT on a Hot Tin Roof
Michigan healthcare freedom community forum
Hospitals continue to consolidate into health systems which have and use their pricing power to increase medical costs well beyond inflation rates and also drive down the wages of medical workers. From the recent HHS Consolidation in Health Care Markets RFI Response:
"In 1990, 65% of Metropolitan Statistical Areas (MSAs) in the country were considered highly concentrated for hospital services; by 2006, the share had increased to 77%, and by 2016, it was 90%. Consolidation trends have continued to this day. A study of 183 MSAs found that between 2017 and 2021, hospital system concentration rose in nearly 70% of MSAs and prices rose in 98%."
This pricing power is now attracting the private equity vultures who are always seeking above market returns. Those above market returns come directly out of your health care insurance premiums and unreimbursed medical costs.
Peter Pitts discusses the baleful influence of hospital consolidations in a RealClearHealth opinion piece, using ProPublica's Sick in A Hospital Town Series as an exemplar:
https://www.realclearhealth.com/articles/2025/12/15/the_hospital_that_swallowed_albany_1153474.html
https://projects.propublica.org/albany-georgia-hospital/
The Hospital that Swallowed Albany
By Peter Pitts - December 15, 2025In Albany, Georgia, the troubling rise of Phoebe Putney Health System (PPHS) is a four-alarm warning. ProPublica’s series “Sick in a Hospital Town” shows how one system can grow with no real checks or balances, shaping care to its own commercial interests by leveraging local politics and the local economy. This is a story about a national bellwether. Hospitals keep merging keep across the country while those responsible for stopping bad deals often stand back. PPHS began as a small-town hospital. Now it runs almost every health care service in the area, and the trend is coming to a hospital near you.
A key question is, why do so few federal enforcement actions target hospital mergers? Why do federal watchdogs let so many hospital deals slide while they tear apart other health care mergers? The Federal Trade Commission (FTC) and the Department of Justice (DOJ) both have clear power to fight hospital mergers, yet they rarely use it. One industry review found that out of more than a thousand hospital mergers in two decades, the FTC challenged only about 1%—even though 20% showed clear warning signs for harm to competition. That is more than a missed chance. It is a pattern that makes patients, employers, and taxpayers pay more for care that often does not improve post-acquisition.
The truth is a harsh mistress, and the data tell a blunt story. After hospital mergers, prices rise. A meta-analysis by the American College of Surgeons found that in 93% of cases, hospital charges went up after a merger. Another study found that prices rose by an average of 1.6% in the first two years after a merger and when hospitals in different markets joined forces, prices jumped almost 13% over six years. These are not small shifts. For families already strained by health bills, every extra dollar hits hard.
Backers of hospital mergers often promise lower costs and better care. The record does not support that claim. Studies show that mergers raise costs or leave them stuck at the same high-water mark. Bluntly put, real gains in quality rarely follow mergers. The reality is that patients are left with fewer real choices and local doctors lose their professional independence. The Albany situation, as ProPublica showed, is instructive. Phoebe Putney’s grip leaves patients with nowhere else to turn. PPHS dominance controls local politics and makes it hard for anyone in town to push back.
Meanwhile, other parts of our healthcare system face far more robust regulatory oversight. When insurance firms or pharmaceutical companies try to merge, regulators often jump in – publicly and aggressively. They hold hearings, demand changes, and often block deals outright. We have to ask ourselves, why do other mergers in the health care space get intense review while hospitals get a free pass, leading to higher costs for consumers, employers, and government programs? Part of the answer sits in how hospitals frame their work. They say they serve the public good, and in many ways they do, but that claim should not shield them from the rules that keep quality high, markets fair, and prices in check. In a recent Washington Times piece, Michael Toth warns of what can happen when leaders act as if the system is in safe and steady hands. It’s not.
The stakes keep rising. Case in point -- private equity firms now see hospitals as prime targets. In early 2025, private equity health care deals hit a new high even as lawmakers in more than a dozen states pushed for stricter oversight. Some states, like Massachusetts, now force hospitals to report deals before they happen. But state action can only go so far. Without strong federal enforcement, hospital systems will keep on growing, local towns will keep losing control, healthcare professionals will lose their ability to practice medicine as they see fit, and patients will suffer the consequences.
Not surprisingly, the American Hospital Association pushes back against reality, claiming that the research is flawed or biased, but the proof is in the pudding. Hospital consolidation raises prices and cuts choice. Fortunately, after years of weak action, the FTC has begun to take notice, recently blocking a hospital deal in North Carolina and updating its merger rules.
If we want to ensure patient access to high quality hospital services, we need to ask hard questions. Why do hospital mergers still get a pass when the costs and consequences sit in plain view? Why do regulators act only after the damage is done? The story of Albany, Georgia, should serve as a blunt wake-up call. When one hospital system controls a town, everyone pays the price.
It's time for federal regulators to step up. Patients deserve real competition, fair prices, and a health care system that puts their needs first. We should not wait for another town to lose its choices before we act.
Peter J. Pitts is President of the Center for Medicine in the Public Interest and a former FDA Associate Commissioner.
So why have hospitals - and the health care industry in general - consolidated?
https://juniperresearchgroup.substack.com/p/how-obamacare-raised-health-care
How Obamacare Raised Health Care Costs
Why can't the Left admit the obvious...?
By Chris Jacobs - December 18, 2025Last week, I testified at a joint hearing of two House Oversight subcommittees discussing health care policy. A full copy of my testimony is available here, but I wanted to highlight a revealing admission made by the minority witness. In addition to advocating for an extension of the enhanced Obamacare subsidies, Sophia Tripoli of Families USA included the following section in her written testimony analyzing the forces driving increases in health care spending:
Hospitals, health systems and other providers have rapidly consolidated, via horizontal and vertical integration, into large health care corporations, amassing outsized market power in order to increase prices for hospital care year after year. In fact, over 1,500 hospital mergers have occurred between 1998 and 2017, with an estimated 40% of those mergers taking place from 2010 to 2015. Moreover, between 2013 and 2021, the percentage of physician practices that were hospital-owned rose from 15% to 53%, and the percentage of physicians employed by a hospital rose from 27% to 52%. [Emphasis added.]
A sizable number of hospital mergers took place between 2010 and 2015? Gee, I wonder if Congress passed any laws in 2010 that might have created this wave of hospital consolidation…
Ms. Tripoli’s comments echo those of Sen. Elizabeth Warren (D-MA), who just over two years ago co-authored a letter noting that medical loss ratio (MLR) regulations have encouraged insurers to buy up pharmaceutical benefit managers and other entities, so they can shift profits from their insurance business (where the MLR caps their profits) to their pharmacy, PBM, or other businesses where profits are uncapped.
Like Ms. Tripoli, Sen. Warren didn’t mention the fact that Obamacare created the MLR requirement that has encouraged this consolidation within the health care sector. Perhaps the Left would have slightly more credibility arguing for an extension of enhanced Obamacare subsidies if they would come out and admit those enhanced subsidies are necessary only because the law underlying them has failed…
Get MHF Insights
News and tips for your healthcare freedom.
We never spam you. One-step unsubscribe.