- ¿Qué tan bajo se puede llegar? Las cambiantes guías para el control de la presión arterial
- Rising Health Costs Push Some Middle-Aged Adults To Skip the Doc Until Medicare
- Even With Dental Insurance, You Still Could Face a Large Bill
- Don't Forget This: Study Shows Cannabis Exacts a Toll on Your Memory
- Want To Stress Less? Start With These Everyday Habits
- Journalists Shine Light on Out-of-Reach Insurance Prices, AI’s Role in Claims Disputes, and Susie Wiles
- Arizona behavioral health center adds 10 adolescent beds
- The explosion of the Medicare Advantage special needs plan
- The explosion of the Medicare Advantage special needs plan
- We’re Great Thinkers…But Not Rethinkers
- North Star to cut additional jobs
- North Star to cut additional jobs
- Oregon Governor asks PeaceHealth to delay contract switch: 11 things to know
- 6 Optum updates to know from Q1
- Viewpoint: US nursing workforce faces several risks
- The shifting dental hygiene landscape
- 12 dental insurance updates in 30 days
- ‘The 1980s called’: CMS to phase out fax, mail
- ‘The 1980s called’: CMS to phase out fax, mail
- Aligning IT & clinical teams: How to reduce friction and improve communication
- AI tool targets billing gaps at Kentucky system
- AI in pharmacy: Why pilots stall at hospitals
- 37 recent hospital, health system executive moves
- This ASC startup is wiring AI into the fabric of outpatient surgery
- Springer Nature retracts 38 papers over autism dataset
- Intermountain plans new outpatient clinic
- Legacy Health, Regence BCBS face looming contract expiration
- Meet the COOs of the largest DSOs
- Michigan bills target outpatient fees, CON requirements
- Anesthesia group, lawmakers oppose Medicare cuts to non-opioid pain treatment
- Iowa lifts emergency suspension of transplant surgeon’s license
- Vascular center, physician CEO to pay $4M to settle fraud allegations
- In the Affordability Alphabet Soup of the ACA and EHBs, a Link to Higher Premiums Isn’t Clear-Cut
- 5 cardiologists stepping into leadership roles
- New York organizations partner on intellectual, developmental disabilities campus
- Cincinnati hospital acquires outpatient center for $6M
- CMS final rule aims to axe the fax machine, phase out paper mailing
- 24 profitable health systems in 2025
- How 2 CFOs plan for uncertainty
- Heartland Dental expands with Texas affiliation
- MD Anderson opens colorectal cancer center
- SALT Dental Partners adds Washington practice
- 11 dental school updates to know
- 6 health systems seeking revenue cycle executive directors
- Remarks at The SEC Speaks in 2026: From Kitchen Table to Cap Table—Making Capital Formation Work for Small Businesses
- Integrated care model drives 76% depression improvement in 44 days: Study
- Heart Benefits From GLP-1 Drugs Fade After Stopping, Study Finds
- Survey Shows More People Struggling To Afford ACA Insurance
- Up to 155,000 COVID Deaths May Not Have Been Counted, Study Finds
- FDA Drops Plan To Ban Tanning Beds for Minors Nationwide
- Idaho bill proposes consolidating dental regulatory oversight
- Washington hospital charts path to preserve primary care
- 4 DSOs making headlines
- 6 state behavioral health policy updates
- 80% of returning ACA enrollees report higher healthcare costs in 2026
- Fitch downgrades HonorHealth’s credit rating
- NYC Health + Hospitals names dentistry, oral surgery leaders
- Mindray North America Enters Ventilator Market
- Mindray North America Enters Ventilator Market
- LivaNova Receives FDA Premarket Approval for to treat Moderate to Severe Obstructive Sleep Apnea
- LivaNova Receives FDA Premarket Approval for to treat Moderate to Severe Obstructive Sleep Apnea
- Perfuze Receives FDA 510(k) Clearance for Millipede88 Aspiration Catheter
- Perfuze Receives FDA 510(k) Clearance for Millipede88 Aspiration Catheter
- EPA proposes new rule on Ethylene Oxide Emissions: Could Loosen Limits on Medical Device Sterilization
- EPA proposes new rule on Ethylene Oxide Emissions: Could Loosen Limits on Medical Device Sterilization
- With Novo's semaglutide going off patent, Indian drugmakers set to launch their cheaper generics
- Sanofi backs 2 more documentary films about rare blood disorders
- ACIP member's miscommunication on vaccine panel's future adds to confusion after court ruling
- Rhythm's Imcivree scores 'transformative' FDA approval in brain damage-related obesity
- Some Patients With ADHD and Addiction History Missing Out
- Social Media Poses Risks to Children's Mental Health, Review Concludes
- 'Early Bird' Exercisers Get The Most Health Benefits, Study Finds
- Does Closing Your Eyes Help You Hear Better?
- High Blood Pressure Deaths Quadruple Among Young Women, Study Finds
- Meningitis Vaccine Doesn't Protect Gay, Bisexual Men From Gonorrhea, Clinical Trial Concludes
- Listen: Trump’s NIH ‘Reset’ Is Driving Away Scientists
- ‘How Low Can You Go?’ The Shifting Guidelines for Blood Pressure Control
- Oz Escalates Medicaid Fraud Claims Against States After Focus on Minnesota
- Mississippi to fund clinical trials for psychedelic drug
- Lawmakers push bill to boost mental health workforce, diversity
- Florida State partners with behavioral health provider on research
- Utah governor signs hygienist autonomy bill
- UHS CEO: Talkspace deal builds 1st national ‘end-to-end’ behavioral model
- Psychedelic therapy shows no benefit over antidepressants: Study
- What the Health? From KFF Health News: RFK Jr.’s Vaccine Schedule Changes Blocked — For Now
- Verily banks $300M to accelerate AI road map, transitions to independent company
- KFF: ACA plan enrollees report rising costs for 2026 coverage
- Industry Voices—Stop buying AI tools, start designing AI architecture
- CSL warns of supply shortfall, treatment delays for hemophilia gene therapy Hemgenix
- 10K Corewell Health nurses vote to authorize labor strike
- Providence mulling sale of its health plan amid financial pressures
- Fierce Pharma Asia—World's 1st brain chip nod; AZ's cell therapy bet; Astellas-CytomX breakup
- Gut Microbiome May Take Years to Recover From Antibiotic Use
- Prepared Remarks Before SEC Speaks
- The Art and Science of Materiality
- Capital, Choice, and the Pursuit of Happiness: Remarks at The SEC Speaks in 2026
- Novo's Wegovy HD passes muster under FDA national priority voucher program
- Hospital operations begin 2026 with depressed margins amid low volumes, high labor spend
- The Math Behind Eczema Flare-Ups May Finally Add Up
- Male preconception startup Upstream announces donor-matching platform
- Women's health sector could grow to $600B industry by 2030: PwC report
- Democratic senators detail plans to take on 'Big Insurance'
- Both Types Of Diabetes Increase Dementia Risk
- Aldi Recalls Spinach Bites Over Possible Contamination
- Collegium ponies up $650M to gain ADHD drug Azstarys from Corium
- Maryland bill calls for more transparency in pharma's disease awareness campaigns
- After Alfasigma's GSK licensing deal, Lynavoy picks up FDA nod in rare liver disease
- What To Know About Fatty Liver Disease and Why It’s So Common
- Drug Smoking Linked To Surge In Severe Burn Cases
- Thymus Gland Health May Be Key to Long Life and Fighting Cancer
- Premature Menopause Increases Heart Disease Risk
- U.S. Teen Obesity Hits Record Highs While Efforts to Slim Down Drop
- Pesticide Exposure Before Pregnancy Might Risk Newborn Health
- UPDATED: AstraZeneca to build cell therapy manufacturing hub, R&D center in Shanghai
- Many ACA Customers Are Paying Higher Premiums. Most Blame Trump and Republicans, Poll Finds.
- CDMO Axplora to pump $60M into Italian complex API plant
- Pfizer eyes earlier Talzenna use after phase 3 prostate cancer win
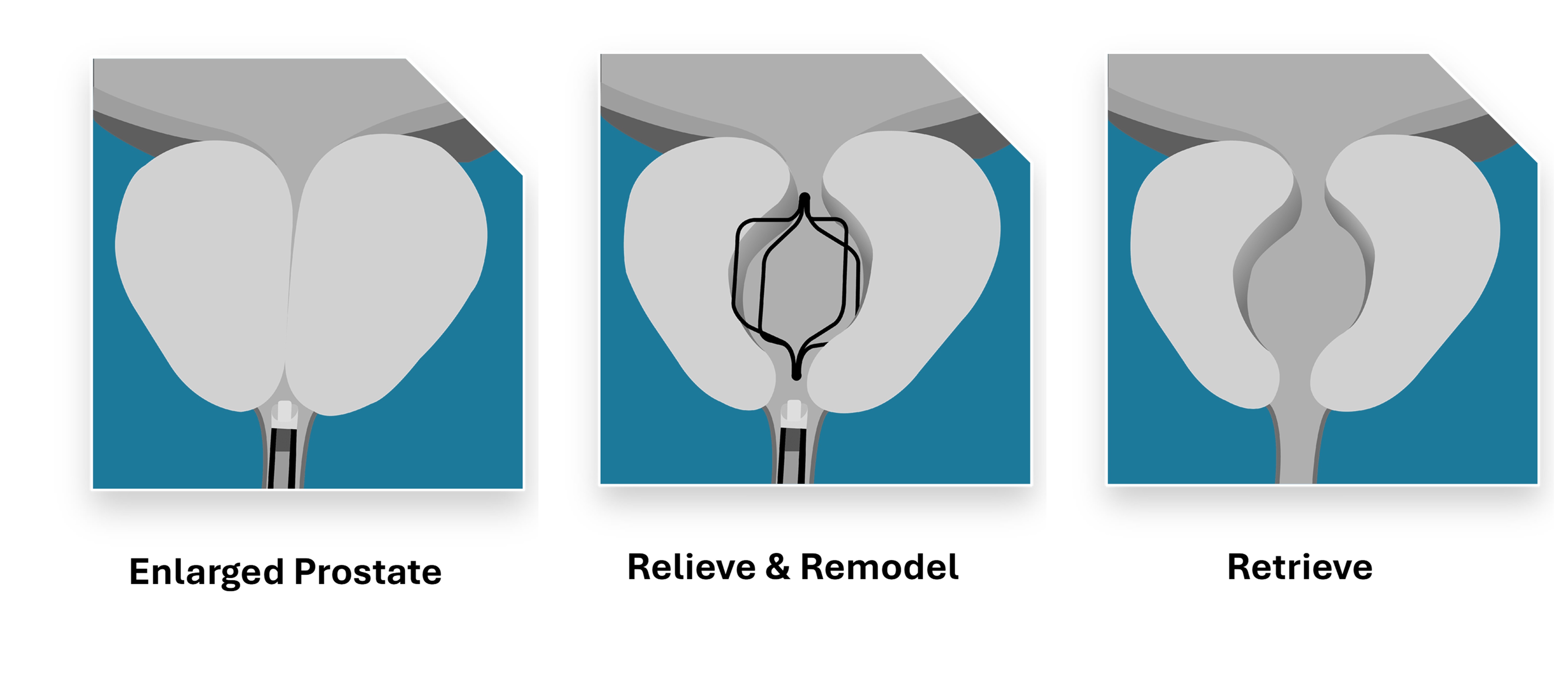
- Prodeon Medical FDA 510(k) approved for the Urocross Expander System, a Non-Permanent Retrievable Implant for Treating Benign Prostatic Hyperplasia
- Prodeon Medical FDA 510(k) approved for the Urocross Expander System, a Non-Permanent Retrievable Implant for Treating Benign Prostatic Hyperplasia
- JenaValve Gets FDA Nod for Trilogy Transcatheter Heart Valve (THV) to Treat Aortic Regurgitation (ssAR)
- JenaValve Gets FDA Nod for Trilogy Transcatheter Heart Valve (THV) to Treat Aortic Regurgitation (ssAR)
- Turquoise Health raises $40M to power healthcare contracts, payments
- To tackle healthcare costs, representatives weigh curbs on provider consolidation
- A look at Highmark's specialty pharmacy partnership with Free Market Health
- AD/PD 2026: New data highlight potential cost-effectiveness of confirmatory AD blood testing in U.S. diagnostic pathways
- With downgrade, HSBC casts doubt about Lilly's 'stairway to heaven' trajectory
- TrumpRx's 'world's lowest' drug price claims fall short in global comparison: NYT
- Study Finds Little Proof Cannabis Helps Most Mental Health Conditions
- Meningitis Outbreak Tied to Students Leaves 2 Dead and 11 Sick in England
- J&J, Protagonist's 'game-changer' once-daily psoriasis pill Icotyde nabs FDA approval
- Belly Fat Linked To Heart Failure Risk
- Women More Likely To Survive Cancer Than Men — At A Cost
- BMS brings 'Emily in Paris' star and cancer survivor Ashley Park aboard campaign honoring oncologists
- Sandoz expands biosim collab with Samsung Bioepis, sets sights on Takeda's Entyvio
- Ultra-Processed Foods Linked To Heart Attack, Stroke, Cardiac Arrest
- E. Coli Outbreak Tied To Raw Cheddar Cheese Sickens 7 People
- The Sunshine Vitamin and COVID: New Study Finds Mixed Results for Recovery
- Too Much Smartphone Use Linked to Disordered Eating in Teens
- Shingles Vaccine Protects Heart Failure Patients From Heart Attack, Stroke
- White House Chief of Staff Susie Wiles Diagnosed With Early Breast Cancer
- Gates-backed TerraPower Isotopes blueprints $450M plant to supply next wave of radiopharmaceuticals
- Regulation Crypto Assets: A Token Safe Harbor
- The Last Chapter in the Book of Howey
- Payers, hospitals pan CMS' plan to bring non-network plans to ACA exchanges
- Optum Real and Suki build out collaboration to tackle payment challenges as R1 teams with AI scribe Heidi
- Indiana homes in on life sciences with $1B growth strategy, plan to create 100K jobs
- Moody's: Insurers' 2026 outlook is negative as cost pressures continue to batter industry
- GSK's management of Flovent allowed it to 'game the system': Hassan
- Allina Health to join Sutter Health in $26B proposed transaction
- Norovirus Sickens Close to 200 People on Caribbean Cruise

You pay for all medical care covered by health care insurance, regardless of whether you use it. Your ever more fantastic health care premiums are a compilation of billings from every field of medicine plagued by fraud, beyond actual health care. City Journal discusses one of today's hot beds of insurance fraud, transgender medicine. News you won't read in the woke MSM:
https://www.city-journal.org/article/insurance-fraud-transgender-medicine
Insurance Fraud Is Widespread in Transgender Medicine
Evidence of billing fraud is fueling a nationwide probe by the Trump administration.
By Leor Sapir - October 30, 2025A key strategy in the Trump administration’s crackdown on gender medicine is identifying and prosecuting insurance fraud. A common form of potential billing fraud involves use of the diagnosis “Endocrine Disorder Not Otherwise Specified” (E34.9 in the International Classification of Diseases handbook), instead of “Gender Identity Disorders” (F64), for patients who do not have or are not being treated for endocrine disorders.
Critics of gender medicine might argue that fraud exists even with appropriate diagnostic coding. The “gender dysphoria” diagnosis, the reasoning goes, was created in 2013 for the purpose of ensuring insurance coverage for medical interventions.
The argument is not without merit. In the 2010s, advocates of gender medicine in the United States recognized the dilemma for their field. Delisting gender identity disorder from the Diagnostic and Statistical Manual of Mental Disorders (DSM) would “destigmatize” gender incongruence, but at the expense of losing insurance coverage, which requires a diagnostic code. Because people who wished to undergo medical transition had no physical pathology, it was not possible to adopt a physiological diagnosis.
Heino Meyer-Bahlburg, a prominent figure in transgender medicine, concluded at the time that “the decision on the categorization of GIV [gender identity variants] cannot be achieved on a purely scientific basis” and called for “a pragmatic compromise.”
The compromise arrived in 2013, when the American Psychiatric Association replaced gender identity disorder with “gender dysphoria” in the DSM-5. Unlike gender identity disorder, the concept of gender dysphoria was not thought to imply that the mismatch between a person’s sex and self-conception of being a man or woman was itself a disorder.
The conceptual problem, however, was not resolved but merely swept under the rug in the interest of working within the constraints of the U.S. health-care system. “The major reason for wanting to keep the diagnosis in the DSM,” wrote Jack Drescher, Peggy Cohen-Kettenis, and Sam Winter, three leaders in the field, “was healthcare reimbursement.”
The World Professional Association for Transgender Health, in its latest “Standards of Care,” recommends the use of “gender incongruence,” a new diagnosis included in the ICD-11 in the category of “Conditions Related to Sexual Health,” as an alternative to the gender identity disorder (F64) codes. The World Health Organization, which publishes the ICD, explained that its inclusion of “gender incongruence” in ICD-11 was intended to “help increase access” to gender transition interventions and “destigmatize the condition.”
Setting aside these criticisms, I will assume for the sake of argument that there is a non-fraudulent diagnostic code for transgender medical procedures (“gender identity disorders,” F64). The problem: plenty of evidence suggests that providers are not using it. Thus, a plausible case can be made that systematic insurance fraud exists.
It’s worth stating up front that transgender identity is not an endocrine disorder, and sex-trait modification (“gender-affirming care”) is not intended to treat any physical pathology.
However, transgender-identified people may develop endocrine disorders as a result of the hormonal or surgical interventions. Consider three examples.
A castrated male will be unable to produce sex hormones, which play a critical role in the maintenance of most body systems. Iatrogenic primary hypogonadism—or doctor-induced underproduction of hormones—results in infertility and can lead to osteoporosis, a serious medical problem.
In its clinical practice guideline on gender medicine, the Endocrine Society recommends that females be given six to 100 times the normal reference range of the virilizing hormones. “Gender-affirming care,” in this case, means iatrogenic hyperandrogenism—an endocrine disorder desired for its secondary cosmetic effects.
A 12-year-old put on gonadotropin-releasing hormone analogues (GnRHa, or “puberty blockers”) will be in a state of iatrogenic hypogonadotropic hypogonadism—an endocrine disorder. Several studies have reported deficiencies of bone mineralization as an expected outcome, increasing in turn the risk for debilitating fractures of the spine and hip. Even when adolescents who are put on GnRHa receive cross-sex hormones, bone mineralization may not catch up to normal levels. (See Section 7.3.2 in the Department of Health and Human Services report on treatment for pediatric gender dysphoria.)
“Gender-affirming care,” in other words, may also be called iatrogenic endocrine disorders, or doctor-induced disorders of sex development (when minors are concerned). If a patient with a normal endocrine system receives “gender-affirming care” and then seeks treatment for the side effects of that “care,” any responsible doctor should treat the patient for that endocrine condition, and billing treatment for an “endocrine disorder” need not constitute fraud, provided the specific, appropriate code is used (see below). A gender clinician who uses the “unspecific” endocrine disorder code, in contrast, raises legitimate suspicion of doing so for a patient who does not currently have an endocrine disorder.
The decision by gender medicine leaders to use endocrine disorder not otherwise specified (E34.9) rather than gender identity disorder (F64) codes, despite the absence of endocrine disorders in people initially seeking gender transition, was a response to Obama-era regulations that required the collection of data on sexual orientation and gender identity in electronic health records; to pressures from transgender-identified patients and their advocates to reduce the stigma associated with “gender identity disorder” diagnoses; and to an insurance landscape in which reimbursement claims for hormones or surgeries were not always fulfilled.
Gender clinicians have also justified the use of E34.9 codes on the grounds that not all people seeking sex trait modification would meet criteria for F64 codes. In 2021, one group of gender clinicians and researchers summarized the matter this way: “The utility of GID [gender identity disorder] codes to identify transgender people is limited by the fact that not all transgender people experience GID and GID codes may be underused by clinicians to avoid labeling the patient as transgender, or to avoid non-payment of insurance claims.”
A WPATH training module from 2021 by Stephen Rosenthal, a pediatric endocrinologist and one of the biggest names in the world of U.S. gender medicine, recommends that clinicians use “Endocrine Disorder” as an alternative to the “Gender Dysphoria” diagnosis when coding for insurance billing.
A 2022 article in KFF Health News titled “Medical Coding Creates Barriers to Care for Transgender Patients” opened with an example of a woman denied insurance coverage for hair removal as part of a phalloplasty procedure (where skin flaps are harvested from the thigh or forearm to create a pseudo-penis). “One reason [for denial of insurance claims] is transphobia within the U.S. health care system,” KFF proclaimed, “but another involves how medical diagnoses and procedures are coded for insurance companies.” Insurance typically does not cover procedures that are considered cosmetic.
Nick Gorton, a gender doctor interviewed for the KFF Health News piece, admitted to using the ICD-10 code for pelvic pain instead of gender-related issues for patients undergoing hysterectomy. Eric Meininger, a pediatrician, acknowledged using the ICD code for “medication management” for “trans kid[s] seeking hormone therapy.” Meininger added, “It’s not hard usually to come up with five or seven or eight diagnoses for someone because there’s lots of vague ones out there.”
In 2023, a JAMIA Open study of health records at the University of Iowa Hospitals and Clinics revealed that 87.5 percent of patients who were put on “gender-affirming therapy” had an endocrine disorder (E34.9) diagnosis in their medical records. The study did not report how many of these patients had that code used for their initial hormone treatment (that is, prior to developing iatrogenic endocrine disorders).
Another 2023 JAMIA Open study, this one of electronic health records at Fenway Health, a community health center in Boston that specializes in transgender medicine, contained an even more dramatic finding. Acknowledging that “Endocrine Disorder Not Otherwise Specified” codes “are frequently utilized to avoid labeling a person as transgender when providing gender-affirming services,” the authors found that, at Fenway Health, “few TGD [transgender/gender-diverse] persons had an ICD code specific to gender identity disorder/dysphoria (ranging from 20.9% to 21.6%). Instead, many TGD individuals had a diagnosis code for an endocrine disorder not otherwise specified (ranging from 60.2% among nonbinary adults assigned female at birth to 82.8% among transgender men).”
In short, the decision by leaders in the field of gender medicine to use “endocrine disorder” codes for patients who lack such disorders was deliberate and is well documented. Indeed, the openness, even pride, with which they discuss this practice shows their confidence that neither the medical establishment nor the insurance industry would dare challenge the field on this critical matter.
It’s hard to know to what extent the experiences of clinics like Fenway are representative of other health-care centers, but some indications suggest that the problem is widespread.
Last year, a Manhattan Institute analysis of an all-payer, all-claims insurance database found an almost 30 percent increase in unspecified endocrine disorder diagnoses among minors between 2020 and 2022. It’s possible that this increase was due to better diagnosis of actual endocrine disorders like central precocious puberty (CPP). But a more likely explanation, given the timeframe, the rarity of CPP, and especially the fact that a specific code for CPP exists (E22.8), is that the increase reflects greater willingness of gender clinicians to use endocrine disorder (E34.9) codes instead of gender identity disorder (F64) codes.
Earlier this month, the Philadelphia Inquirer reported that the U.S. Department of Justice had launched a probe into the Children’s Hospital of Philadelphia and the Children’s Hospital of Pittsburgh after finding potential evidence of billing fraud. Contractors hired by the Trump administration to examine billing practices found evidence that, between 2017 and 2024, hospital officials made 250 diagnoses of CPP in children ages ten and up, “including numerous teenagers aged 14 to 18.” Two days later, the Daily Caller reported on a similar probe into Boston Children’s Hospital after government officials noted that the hospital went from “diagnosing almost no 11-year-olds with CPP for the years 2017–2019 to diagnosing 50 11-year-old patients with CPP in 2022.”
CPP is an endocrine disorder in which puberty appears at an abnormally early age and is treated with puberty blockers. At least some of the patients at CHOP and BCH appear to be well outside the age range for CPP, raising legitimate suspicion of fraudulent billing practices.
The Department of Justice probes into CHOP and BCH are part of a broader federal investigation into health-care institutions that offer sex-trait modification procedures to minors. A Massachusetts court is currently blocking that investigation.
The legal repercussions of billing fraud are potentially dire. Where public insurance (Medicaid) is concerned, it can include criminal charges. Violators may face imprisonment for up to ten years and fines of up to $250,000, as well as other penalties. Civil penalties under the federal False Claims Act include exclusion from federal health-care benefit programs, loss of license, and hefty fines per false claim.
Last week, news broke that May Lau, a gender physician from Texas who had been under investigation by state authorities for violating the state prohibition on pediatric gender transition and disguising her violations with fraudulent billing, agreed to surrender her Texas medical license. Lau has reportedly relocated to Oregon, where she can continue to practice “gender-affirming care” on minors.
It thus remains to be seen whether providers who offer gender transition and use inappropriate diagnostic codes will be held liable for their actions.
Get MHF Insights
News and tips for your healthcare freedom.
We never spam you. One-step unsubscribe.