- Orthopedic ASC proposed in Massachusetts
- Sutter-Allina deal pushes ambulatory growth strategy
- FTC launches healthcare task force
- Meet the CEOs, presidents leading the largest ASC companies
- Algunos adultos de mediana edad deciden posponer la atención médica hasta tener Medicare
- 30K pounds of hospital grown food: How farmers figure into Trinity’s prescriptions
- ¿Qué tan bajo se puede llegar? Las cambiantes guías para el control de la presión arterial
- Even With Dental Insurance, You Still Could Face a Large Bill
- Rising Health Costs Push Some Middle-Aged Adults To Skip the Doc Until Medicare
- FDA solicits feedback on controversial national priority voucher review pathway
- Health Tech Weekly Rundown: Perplexity rolls out AI-powered medical records search; Doximity survey examines how docs use AI
- Don't Forget This: Study Shows Cannabis Exacts a Toll on Your Memory
- Want To Stress Less? Start With These Everyday Habits
- Journalists Shine Light on Out-of-Reach Insurance Prices, AI’s Role in Claims Disputes, and Susie Wiles
- Arizona behavioral health center adds 10 adolescent beds
- The explosion of the Medicare Advantage special needs plan
- The explosion of the Medicare Advantage special needs plan
- We’re Great Thinkers…But Not Rethinkers
- North Star to cut additional jobs
- North Star to cut additional jobs
- Oregon Governor asks PeaceHealth to delay contract switch: 11 things to know
- 6 Optum updates to know from Q1
- Viewpoint: US nursing workforce faces several risks
- The shifting dental hygiene landscape
- 12 dental insurance updates in 30 days
- ‘The 1980s called’: CMS to phase out fax, mail
- ‘The 1980s called’: CMS to phase out fax, mail
- Aligning IT & clinical teams: How to reduce friction and improve communication
- AI tool targets billing gaps at Kentucky system
- AI in pharmacy: Why pilots stall at hospitals
- This ASC startup is wiring AI into the fabric of outpatient surgery
- Springer Nature retracts 38 papers over autism dataset
- Intermountain plans new outpatient clinic
- Legacy Health, Regence BCBS face looming contract expiration
- Meet the COOs of the largest DSOs
- Michigan bills target outpatient fees, CON requirements
- Anesthesia group, lawmakers oppose Medicare cuts to non-opioid pain treatment
- Iowa lifts emergency suspension of transplant surgeon’s license
- In the Affordability Alphabet Soup of the ACA and EHBs, a Link to Higher Premiums Isn’t Clear-Cut
- New York organizations partner on intellectual, developmental disabilities campus
- CMS final rule aims to axe the fax machine, phase out paper mailing
- 24 profitable health systems in 2025
- How 2 CFOs plan for uncertainty
- Heartland Dental expands with Texas affiliation
- SALT Dental Partners adds Washington practice
- 11 dental school updates to know
- 6 health systems seeking revenue cycle executive directors
- Remarks at The SEC Speaks in 2026: From Kitchen Table to Cap Table—Making Capital Formation Work for Small Businesses
- Integrated care model drives 76% depression improvement in 44 days: Study
- Heart Benefits From GLP-1 Drugs Fade After Stopping, Study Finds
- Survey Shows More People Struggling To Afford ACA Insurance
- Up to 155,000 COVID Deaths May Not Have Been Counted, Study Finds
- FDA Drops Plan To Ban Tanning Beds for Minors Nationwide
- Idaho bill proposes consolidating dental regulatory oversight
- Washington hospital charts path to preserve primary care
- 4 DSOs making headlines
- 6 state behavioral health policy updates
- 80% of returning ACA enrollees report higher healthcare costs in 2026
- Fitch downgrades HonorHealth’s credit rating
- NYC Health + Hospitals names dentistry, oral surgery leaders
- Mindray North America Enters Ventilator Market
- Mindray North America Enters Ventilator Market
- LivaNova Receives FDA Premarket Approval for to treat Moderate to Severe Obstructive Sleep Apnea
- LivaNova Receives FDA Premarket Approval for to treat Moderate to Severe Obstructive Sleep Apnea
- Perfuze Receives FDA 510(k) Clearance for Millipede88 Aspiration Catheter
- Perfuze Receives FDA 510(k) Clearance for Millipede88 Aspiration Catheter
- EPA proposes new rule on Ethylene Oxide Emissions: Could Loosen Limits on Medical Device Sterilization
- EPA proposes new rule on Ethylene Oxide Emissions: Could Loosen Limits on Medical Device Sterilization
- With Novo's semaglutide going off patent, Indian drugmakers set to launch their cheaper generics
- Sanofi backs 2 more documentary films about rare blood disorders
- ACIP member's miscommunication on vaccine panel's future adds to confusion after court ruling
- Rhythm's Imcivree scores 'transformative' FDA approval in brain damage-related obesity
- Some Patients With ADHD and Addiction History Missing Out
- Social Media Poses Risks to Children's Mental Health, Review Concludes
- 'Early Bird' Exercisers Get The Most Health Benefits, Study Finds
- Does Closing Your Eyes Help You Hear Better?
- High Blood Pressure Deaths Quadruple Among Young Women, Study Finds
- Meningitis Vaccine Doesn't Protect Gay, Bisexual Men From Gonorrhea, Clinical Trial Concludes
- Oz Escalates Medicaid Fraud Claims Against States After Focus on Minnesota
- Listen: Trump’s NIH ‘Reset’ Is Driving Away Scientists
- ‘How Low Can You Go?’ The Shifting Guidelines for Blood Pressure Control
- Mississippi to fund clinical trials for psychedelic drug
- Lawmakers push bill to boost mental health workforce, diversity
- Florida State partners with behavioral health provider on research
- Utah governor signs hygienist autonomy bill
- UHS CEO: Talkspace deal builds 1st national ‘end-to-end’ behavioral model
- Psychedelic therapy shows no benefit over antidepressants: Study
- What the Health? From KFF Health News: RFK Jr.’s Vaccine Schedule Changes Blocked — For Now
- Verily banks $300M to accelerate AI road map, transitions to independent company
- KFF: ACA plan enrollees report rising costs for 2026 coverage
- Industry Voices—Stop buying AI tools, start designing AI architecture
- CSL warns of supply shortfall, treatment delays for hemophilia gene therapy Hemgenix
- 10K Corewell Health nurses vote to authorize labor strike
- Providence mulling sale of its health plan amid financial pressures
- Fierce Pharma Asia—World's 1st brain chip nod; AZ's cell therapy bet; Astellas-CytomX breakup
- Gut Microbiome May Take Years to Recover From Antibiotic Use
- Prepared Remarks Before SEC Speaks
- The Art and Science of Materiality
- Capital, Choice, and the Pursuit of Happiness: Remarks at The SEC Speaks in 2026
- Novo's Wegovy HD passes muster under FDA national priority voucher program
- Hospital operations begin 2026 with depressed margins amid low volumes, high labor spend
- The Math Behind Eczema Flare-Ups May Finally Add Up
- Male preconception startup Upstream announces donor-matching platform
- Women's health sector could grow to $600B industry by 2030: PwC report
- Democratic senators detail plans to take on 'Big Insurance'
- PrescriberPoint's solution to the modern prescribing journey
- Both Types Of Diabetes Increase Dementia Risk
- Aldi Recalls Spinach Bites Over Possible Contamination
- Collegium ponies up $650M to gain ADHD drug Azstarys from Corium
- Maryland bill calls for more transparency in pharma's disease awareness campaigns
- After Alfasigma's GSK licensing deal, Lynavoy picks up FDA nod in rare liver disease
- What To Know About Fatty Liver Disease and Why It’s So Common
- Drug Smoking Linked To Surge In Severe Burn Cases
- Thymus Gland Health May Be Key to Long Life and Fighting Cancer
- Premature Menopause Increases Heart Disease Risk
- U.S. Teen Obesity Hits Record Highs While Efforts to Slim Down Drop
- Pesticide Exposure Before Pregnancy Might Risk Newborn Health
- UPDATED: AstraZeneca to build cell therapy manufacturing hub, R&D center in Shanghai
- How CVS Caremark Is Shaping the Future of Pharmacy Benefits
- CDMO Axplora to pump $60M into Italian complex API plant
- Pfizer eyes earlier Talzenna use after phase 3 prostate cancer win
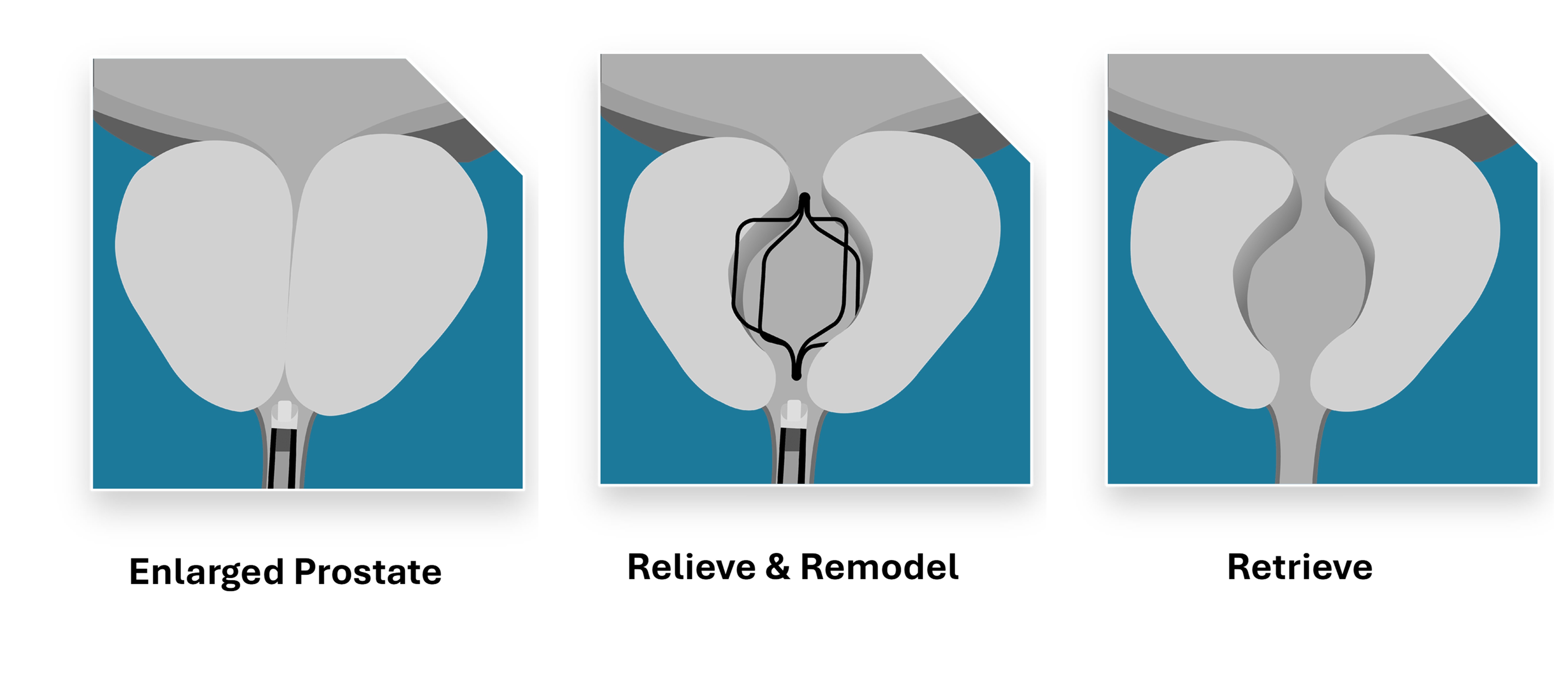
- Prodeon Medical FDA 510(k) approved for the Urocross Expander System, a Non-Permanent Retrievable Implant for Treating Benign Prostatic Hyperplasia
- Prodeon Medical FDA 510(k) approved for the Urocross Expander System, a Non-Permanent Retrievable Implant for Treating Benign Prostatic Hyperplasia
- JenaValve Gets FDA Nod for Trilogy Transcatheter Heart Valve (THV) to Treat Aortic Regurgitation (ssAR)
- JenaValve Gets FDA Nod for Trilogy Transcatheter Heart Valve (THV) to Treat Aortic Regurgitation (ssAR)
- Turquoise Health raises $40M to power healthcare contracts, payments
- To tackle healthcare costs, representatives weigh curbs on provider consolidation
- A look at Highmark's specialty pharmacy partnership with Free Market Health
- AD/PD 2026: New data highlight potential cost-effectiveness of confirmatory AD blood testing in U.S. diagnostic pathways
- With downgrade, HSBC casts doubt about Lilly's 'stairway to heaven' trajectory
- TrumpRx's 'world's lowest' drug price claims fall short in global comparison: NYT
- Beyond payment integrity: An AI-driven approach to affordability
- Study Finds Little Proof Cannabis Helps Most Mental Health Conditions
- Meningitis Outbreak Tied to Students Leaves 2 Dead and 11 Sick in England
- J&J, Protagonist's 'game-changer' once-daily psoriasis pill Icotyde nabs FDA approval
- Belly Fat Linked To Heart Failure Risk
- Women More Likely To Survive Cancer Than Men — At A Cost
- BMS brings 'Emily in Paris' star and cancer survivor Ashley Park aboard campaign honoring oncologists
- healow Genie AI Contact Center Helped Manage 76% of Calls—Demonstrating That Patient Access and Operational Efficiency Go Together
- Sandoz expands biosim collab with Samsung Bioepis, sets sights on Takeda's Entyvio
- Ultra-Processed Foods Linked To Heart Attack, Stroke, Cardiac Arrest
- E. Coli Outbreak Tied To Raw Cheddar Cheese Sickens 7 People
- The Sunshine Vitamin and COVID: New Study Finds Mixed Results for Recovery
- Too Much Smartphone Use Linked to Disordered Eating in Teens
- Shingles Vaccine Protects Heart Failure Patients From Heart Attack, Stroke
- White House Chief of Staff Susie Wiles Diagnosed With Early Breast Cancer
- Gates-backed TerraPower Isotopes blueprints $450M plant to supply next wave of radiopharmaceuticals
- Regulation Crypto Assets: A Token Safe Harbor
- The Last Chapter in the Book of Howey
- Payers, hospitals pan CMS' plan to bring non-network plans to ACA exchanges

Today is the deadline to sign a 2026 PPACA-compliant health insurance policy plan. Sales of these plans in Michigan will be off 7.5%:
40,000 fewer Michiganders seek Affordable Care Act health insurance
By Eli Newman - January 14, 2026
- About 40,000 fewer Michiganders are signing up for Affordable Care Act health insurance plans this year
- Rising premiums and the expiration of tax subsidies are contributing to rising prices for coverage
- The open enrollment deadline is Thursday
About 40,000 fewer Michiganders are signing up for Affordable Care Act health insurance plans this year, according to new federal data, following a national trend in people dropping coverage amid rising premiums and expiring subsidies.
The Centers for Medicare & Medicaid Services reports 491,565 Michigan residents signed up through HealthCare.gov or have been automatically renewed in plans since the start of the 2026 marketplace open enrollment period in November. The agency reported 531,083 people in the state had selected plans at the same time last year.
Ahead of Thursday’s open enrollment deadline, policy analysts and health care stakeholders in Michigan pointed to several reasons for the rise in health insurance rates this year, including Congress’s failure to extend ACA-tax credits for premiums.
Still, state insurance regulators say the “biggest mistake” would be missing the opportunity to get health insurance coverage this year.
“Comprehensive, high-quality health insurance leads to better health outcomes, and time is running out for consumers to take advantage of free, local assistance to get the coverage they need through the Health Insurance Marketplace,” said Michigan Department of Insurance and Financial Services Director Anita Fox in a statement earlier this month.
Nationally, around 800,000 fewer people have selected plans compared to a similar time last year, marking a 3.5% drop in total enrollment so far. That includes a decrease in both new consumers signing up for ACA plans and existing enrollees re-upping them.
The new data released Monday evening by the Centers for Medicare and Medicaid Services is only a snapshot of a continuously changing pool of enrollees. It includes sign-ups through Jan. 3 in states that use Healthcare.gov for ACA plans and through Dec. 27 for states that have their own ACA marketplaces. In most states, the period for shopping for plans continues through Thursday for plans that start in February.
But even though it’s early, the data builds on fears that expiring enhanced tax credits could cause a dip in enrollment and force many Americans to make tough decisions to delay buying health insurance, look for alternatives or forgo it entirely.
Experts warn that the number of people who have signed up for plans may still drop even further, as enrollees get their first bill in January and some choose to cancel.
At an appearance in Detroit Tuesday, President Donald Trump promised to unveil a new “health care affordability framework” later this week that he promised would lower the cost of care. He also pledged to soon offer more plans to help with affordability nationwide — even as he blamed Democrats for hyping up the issue.
“One of our top priorities of this mission is promoting greater affordability. Now, that’s a word used by the Democrats,” Trump said. “They’re the ones who caused the problem.”
In reaction to the federal government’s figures, Protect Our Care Michigan director Dianne Byrum laid the blame at the hands of the GOP in Washington.
“The solution is clear and already passed the House: a clean, three-year extension of the ACA tax credits. The only things standing in the way are Senate Republicans and Donald Trump,” she said in a statement.
Michigan's final PPACA plan enrollment on HealthCare.gov was 497,064 in the just concluded 2026 insurance purchasing window. This is down 6.4% from the comparable 531,083 enrollment during 2025. No way to determine how many of these enrollees are phantoms:
Marketplace 2026 Open Enrollment Period Report: National Snapshot
Affordable Care Act Marketplace 2026 Open Enrollment Period Report: National SnapshotThe Centers for Medicare & Medicaid Services (CMS) reports that 23.0 million consumers have signed up for 2026 individual market health insurance coverage through the Marketplaces since the start of the 2026 Marketplace Open Enrollment Period (OEP) on November 1, 2025. This includes 15.8 million Marketplace plan selections in the 30 states using the HealthCare.gov platform for the 2026 plan year and 7.2 million plan selections in the 20 states and the District of Columbia with state-based Exchanges (SBEs) that are using their own eligibility and enrollment platforms.[1] Total nationwide plan selections include 3.4 million consumers who are new to the Marketplaces for 2026, and 19.6 million consumers who had active 2025 coverage and selected a plan for 2026 coverage or were automatically re-enrolled. Open Enrollment on HealthCare.gov ran through January 15, 2026. State-based Exchange enrollment deadlines vary.
Definitions and details on the data in this report are included in the glossary.
Exchange and Consumer Type
Cumulative 2026 OEP Plan Selections
Total: All Exchanges
22,973,219New Consumers
3,382,189Returning Consumers[2]
19,591,030Total: HealthCare.gov
15,771,397New Consumers
2,517,617Returning Consumers
13,253,780Total State-based Exchanges[3]
7,201,822New Consumers
864,572Returning Consumers
6,337,2502026 Marketplace Open Enrollment Period Plan Selections by State
(New Consumers and Returning Consumers)State
Platform
Cumulative 2026 OEP Plan SelectionsAlabama
HealthCare.gov
455,776Alaska
HealthCare.gov
26,079Arizona
HealthCare.gov
357,144Arkansas
HealthCare.gov
160,307California
SBE
1,910,476Colorado
SBE
266,988Connecticut
SBE
150,719Delaware
HealthCare.gov
44,663District of Columbia
SBE
15,323Florida
HealthCare.gov
4,538,772Georgia
SBE
1,301,254Hawaii
HealthCare.gov
23,380Idaho
SBE
120,426Illinois
SBE
441,657Indiana
HealthCare.gov
300,049Iowa
HealthCare.gov
123,304Kansas
HealthCare.gov
192,811Kentucky
SBE
86,297Louisiana
HealthCare.gov
296,648Maine
SBE
57,456Maryland
SBE
248,770Massachusetts
SBE
385,361Michigan
HealthCare.gov
497,064Minnesota
SBE
134,825Mississippi
HealthCare.gov
313,392Missouri
HealthCare.gov
365,734Montana
HealthCare.gov
73,255Nebraska
HealthCare.gov
128,492Nevada
SBE
100,840New Hampshire
HealthCare.gov
66,024New Jersey
SBE
493,816New Mexico
SBE
80,163New York
SBE
208,040North Carolina
HealthCare.gov
761,457North Dakota
HealthCare.gov
41,014Ohio
HealthCare.gov
469,616Oklahoma
HealthCare.gov
261,887Oregon
HealthCare.gov
118,372Pennsylvania
SBE
482,183Rhode Island
SBE
38,071South Carolina
HealthCare.gov
587,567South Dakota
HealthCare.gov
50,951Tennessee
HealthCare.gov
569,310Texas
HealthCare.gov
4,172,233Utah
HealthCare.gov
387,336Vermont
SBE
30,399Virginia
SBE
365,787Washington
SBE
282,971West Virginia
HealthCare.gov
55,879Wisconsin
HealthCare.gov
291,336Wyoming
HealthCare.gov
41,545Glossary
HealthCare.gov: The 30 states that use the HealthCare.gov platform for the 2026 coverage year include: Alabama, Alaska, Arizona, Arkansas, Delaware, Florida, Hawaii, Indiana, Iowa, Kansas, Louisiana, Michigan, Mississippi, Missouri, Montana, Nebraska, New Hampshire, North Carolina, North Dakota, Ohio, Oklahoma, Oregon, South Carolina, South Dakota, Tennessee, Texas, Utah, West Virginia, Wisconsin, and Wyoming.
State-based Exchanges (SBEs): The Exchanges in the 20 states and the District of Columbia that operate their own eligibility and enrollment platforms. The 21 SBEs for 2026 include: California, Colorado, Connecticut, the District of Columbia, Georgia, Idaho, Illinois, Kentucky, Maine, Maryland, Massachusetts, Minnesota, Nevada, New Jersey, New Mexico, New York, Pennsylvania, Rhode Island, Vermont, Virginia and Washington. Generally, the data metric definitions provided here are applicable to the SBE metrics, with some exceptions. Please contact the SBEs for additional information on their metrics.
Cumulative Plan Selections: The cumulative metric represents the total number of people who have submitted an application and selected a plan, net of any cancellations from a consumer or cancellations from an insurer that have occurred from November 1, 2025, through the end of the reporting period. To have their coverage effectuated, consumers generally need to pay their first month’s health plan premium, if applicable. This release does not report the number of effectuated enrollments.
New Consumers (HealthCare.gov): Consumers are considered new if they did not have 2025 Marketplace coverage through HealthCare.gov through December 31, 2025, and made a 2026 plan selection through the federal platform.
New Consumers (SBEs): Consumers are considered new if they did not have 2025 Marketplace coverage in the SBE that uses its own platform where they made a 2026 plan selection through the SBE.
Returning Consumers (HealthCare.gov): Consumers are considered returning if they have 2025 Marketplace coverage through HealthCare.gov through December 31, 2025, and either actively select the same plan or a new plan for 2026. The returning consumers’ count includes consumers who have been automatically re-enrolled in their current plan for 2026 coverage.
Returning Consumers (SBEs): Consumers are considered returning if they have 2025 Marketplace coverage through December 31, 2025, in the same SBE where they actively select the same plan or a new plan for 2026. The returning consumers’ count includes consumers who have been automatically re-enrolled in their 2025 plan or an alternative suggested plan for 2026 coverage.
This communication was printed, published, or produced and disseminated at U.S. taxpayer expense.
The Hill brings us the national story. Experts are predicting myriad recisions during 2026 due to the much higher, less subsidized plan prices:
https://thehill.com/policy/healthcare/5712648-obamacare-enrollment-drops-subisides-expiration/
ACA enrollment drops by 1M-plus after subsidies expire
By Ashleigh Fields - January 29, 2026Affordable Care Act (ACA) enrollment dropped by more than a million after enhanced subsidies expired last year, causing monthly insurance premiums to skyrocket.
The Centers for Medicare and Medicaid Services (CMS) reported Wednesday that 23 million people signed up for open enrollment, which concluded on Jan. 15. It marks a drop-off from the 24.2 million people who enrolled for insurance during the same period in 2025.
Last year marked four consecutive years of record enrollment for ACA Marketplace plans. Gains were credited to enhanced premiums tax credits signed into law under former President Biden through the American Rescue Plan and extended by the Inflation Reduction Act.
Heightened prices reflect the expiration of the COVID-19 pandemic-era tax credits, which kept health insurance costs lower for struggling Americans. The issue was a major flashpoint in spending talks last year, and the turmoil resulted in a 43-day record-long government shutdown.
Democratic lawmakers have pushed for a three-year extension of the subsidies, but the House-passed bill has stalled in the Senate.
Health care advocates have decried the decision to allow premiums to skyrocket, citing harsh conditions that may require citizens to choose between food and medical care.
“Having folks get off the system will derail the entire health care marketplace, especially as more people will unenroll after they receive their first bill,” Rep. Adam Smith (D-Wash.) said in a statement this week, noting thousands in his home state are now uninsured because they “cannot make ends meet.”
His concerns were echoed by Kevin Patterson, CEO of Connect for Health Colorado, who said he’s seeing similar drop-offs.
“On one hand, it’s encouraging to see enrollment remain relatively steady, with only a slight dip, and to see so many people receive meaningful financial assistance,” Patterson said in a statement. “On the other hand, it’s deeply troubling that a record number of people are canceling their plans because they simply can’t afford their monthly payments, or are being forced to choose between health care and basic necessities like housing and food.”
He added, “Without federal enhanced Premium Tax Credits, this alarming trend is, sadly, emerging across the country.”
The latest numbers reflect the data from the 30 states that use the federal ACA Marketplace. Some states that rely on their own independent exchanges have open enrollment until later this week, which could affect the enrollment numbers.
“These numbers are going to go dramatically down month after month as people decide that they can’t afford health care and stop paying their premiums,” Leslie Dach, chair of Protect Our Care, an advocacy group, said in a statement, according to CNN.
Get MHF Insights
News and tips for your healthcare freedom.
We never spam you. One-step unsubscribe.