- Eli Lilly’s 340B deadline passes: What hospitals should know
- OpenEvidence: 6 things to know about the AI tool used by half of physicians
- 29 behavioral health executive moves to know
- Sutter Health’s Epic command center adds 12 beds a day
- 3 states where dental hygienist pay dropped
- 5 states where dental assistant pay dropped
- ‘Absurd’ or the future? Health system leaders weigh in on AI physicians
- Hospital closure slowdown masks a bigger threat ahead
- Illinois nurses union sues Prime, Ascension over alleged understaffing
- Geisinger names director of venture capital arm
- New Jersey hospital CEO to retire
- Judge strikes down $100K H-1B visa fee: 6 notes
- Lee Health names next CEO
- ‘No disruptions’: Elevance study backs take-home methadone
- From financial crisis to acquisition: How the $3.9B Ascension-AmSurg deal unfolded
- Federal workforce programs boost dental care accessibility: 5 notes
- Ultradent acquires dental laser manufacturer
- How a routine Medicare form became a 33-month fraud conviction
- ADA Forsyth Institute ranks among top research institutions
- HST Pathways inks investment
- New York names first-ever freestanding ASC representative to state council
- The Stark law case every physician employer should be paying attention to right now
- Dartmouth Health targets treatment gap for pregnant patients with SUD
- U of Buffalo to end oral surgery residency program
- How Texas became one of the hottest ASC markets in the country
- From affordability to engagement, these are the topics to watch at AHIP 2026
- 13 state behavioral health policy updates
- 5 hospitals, health systems investing in GI
- Accrediting bodies, more medical schools commit to RFK Jr.'s nutrition education pledge
- Children's Well-Being Plummets Across 29 States, Report Finds
- 6 states grant cross-state counseling privileges
- Where the future of teledentistry is headed next
- The payer tactics hurting ASCs most
- 5 red flags in an ASC partnership agreement
- Stamford Health plans $275M cancer, behavioral health expansion
- Federal autism advisers back assisted spelling despite scientific criticism
- Senate HELP committee chairman seeks info on NYC Health + Hospital data breach
- 10 most-viewed psychiatry residency programs in 2025
- 7 dentists making headlines
- ADA: Lilly posts oral semaglutide-topping data as Foundayo speeds toward 2nd potential nod in diabetes
- With ADA in the books, analyst says Lilly is ‘widening its lead’ in the obesity race
- Former clinic CEO pleads guilty to filing false tax returns
- CVS launched an AI Learning Academy for its workforce. Here's why
- Just 5 Minutes Of Prayer Helps Reduce Pain and Anxiety, Study Finds
- Sophia Genetics, Memorial Sloan Kettering sign strategic collab for AI-powered precision oncology hub
- ‘Law & Order’ star Mariska Hargitay teams up with BMS to investigate multiple myeloma research in awareness campaign
- Medtronic Advances Hugo Robotic Surgery Platform with Key FDA Filings and Product Approvals
- Medtronic Posts Strongest Revenue Growth in a Decade, Driven by Cardiovascular and Surgical Businesses
- ADA: Novo's Wegovy pill reaches new GLP-1 patients with impressive 3M prescription milestone
- Boston Scientific Plans Indiana Distribution Center, 300 New Jobs
- Cities sue Trump administration to block final ACA rule
- Irregular Sleep Risks Preschool Kids' Brain Power
- Why Alcohol Makes You Crave Salty Snacks — And How Protein-Rich Foods Can Help Prevent Weight Gain
- ADHD ‘Masking’ May Help People Blend In But Harms Mental Health
- Getting The RSV Shot, Abrysvo, While Pregnant Could Protect Your Baby After Birth
- Pfizer scores FDA pediatric expansion for hemophilia treatment Hympavzi
- Upcoming Billing Change Could Make Pregnancy Pricier
- MAHA’s Treatments for Autism: Camel’s Milk, Stem Cell Injections — And Spelling Therapy
- By September, Nearly a Third of Americans Will Live in States With Legal Aid in Dying
- Hikma earmarks $267M to expand pair of Ohio production sites, add 350 jobs
- Stepful banks $55M to scale AI-powered medical training to boost the workforce pipeline
- ADA: Amgen highlights Repatha perks, GLP-1 pitfalls in push to boost cardiometabolic pedigree
- Gounder Fills In Details Behind Ebola, GLP-1, and Trump Headlines
- Untreated Cancer, Festering Infections: Immigrant Detainees Detail Medical Care Lapses
- Elation Health acquires Aster as it ramps up agentic AI for primary care
- Virginia dental practice suffers data breach affecting 5,200 individuals
- Virginia oral surgery practice suffers data breach affecting 7,000 individuals
- States ranked by mental health social workers per capita
- New York opens 60-bed OUD recovery center
- Dengue Is No Longer Just A Travel Risk — What Google’s Mosquito Plan Could Mean For Your Summer
- Brain Surgery For Pituitary Tumor Helps Illinois Mom Have Second Baby
- Essence Healthcare, Oura expand partnership to sleep apnea detection
- Takeda takes $2.5B legal charge after pay-for-delay verdict, swings to loss for '25
- Industry Voices—A healthcare experience that is as seamless as it is soulful
- Fullspan Health debuts Healthline AI companion to connect consumers to medical content and providers
- As pro-life pressure ramps up on Trump, FDA is investigating safety of abortion pill: WSJ
- As pro-life pressure ramps up on Trump, FDA is investigating safety of abortion pill: WSJ
- Popular Blood Pressure Meds, Dihydropyridine Calcium-Channel Blockers, Linked To Kidney Damage Risk In Type 2 Diabetes
- Too Much Sitting In Pregnancy Doubles Risk Of Complications
- Spinal Cord Stimulation May Restore Arm Strength After Stroke
- Behind the headlines of ASCO 2026
- RFK Jr. Seeks To Peek At Americans' Medical Records For Clues On Autism And Vaccines
- Two-Pill Combo, Inqovi and Venclexta, Offers Hospital-Free Leukemia Treatment Option For Older Adults With AML
- ‘We Live With Fear’: In Congo, Doctors Face Ebola With Little Protection
- Millions of Kids Could Lose Insurance as GOP Healthcare Cuts Start To Bite
- Upcoming Billing Change Could Make Pregnancy Pricier
- WellSpan Health strikes strategic partnership with Philips to deploy, co-develop new healthcare tech
- At first public hearing for FDA’s CNPV program, industry support meets ‘deep concern’ from experts
- “Harmonization: We’ll Have Lots to Talk About”
- Remarks at the Investor Advisory Committee Meeting
- A Quarter for your Thoughts: Remarks at the Meeting of the SEC Investor Advisory Committee
- Weekly Rundown: Trump signs AI executive order; Health Catalyst to sell Vitalware for $147M
- Small businesses feel the squeeze as healthcare costs rise: Morgan Health
- Poll Finds Broad Support For Stricter Regulations On Ultra-Processed Foods
- It's unanimous: SCOTUS agrees with Hikma in 'skinny label' case vs. Amarin
- Remarks at the Investor Advisory Committee Meeting
- Fierce Pharma Asia—China's biotech rise; ASCO highlights; Lilly pipeline deals
- Nearly 1 in 5 Young People Turn to AI Chatbots for Mental Health Advice
- Ixlayer rolls out digital acute pain management platform in collaboration with Vertex Pharmaceuticals
- Ixlayer rolls out digital acute pain management platform in collaboration with Vertex Pharmaceuticals
- Georgetown study: 2M children have dropped out of Medicaid, CHIP since January 2025
- ScionHealth sends 8 community hospitals to Lifepoint Health
- ADC Therapeutics' shares plummet after patient deaths in trial of Zynlonta
- As China biotech crackdown calls reverberate in Washington, the pushback gets louder, too
- Older LGBTQ+ Adults Fear Less Support As They Age, Poll Shows
- Night Owls Are More Prone To Anxiety, Loneliness
- Home-Delivered Medical Meals Reduce ER Visits, Save Money
- Axsome fends off generic competition to narcolepsy med Sunosi until 2040
- Menopause Hormone Therapy Use Drops Sharply Across United States
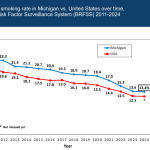
- Michigan Found A Way To Reduce School Vaccine Waivers — Until It Backfired
- Listen to the Latest ‘KFF Health News Minute’
- Louisiana’s Reporting Law Chills Immigrant Medicaid Applications
- RFK Jr. Seeks To Peek at Americans’ Medical Records for Clues on Autism and Vaccines
- Medline earns FDA warning letter ire for repeated toxic bacteria problems
- 8 Requirements for AI Medical Interpreting: 2026 Survey Results
- Healthcare Dealmakers—WakeMed to join Atrium Health, Qualtrics closes $6.8B Press Ganey deal and more
- Millions on Medicaid May Soon Have To Prove They’re Working To Keep Coverage
- Anomaly Insights launches AI solution for managed care executives
- Lilly, Boehringer to slash at least $1B each from planned investments in Germany
- Just 90 Minutes Of Strength Training A Week Linked To Longer Life
- Amid Miplyffa launch, Zevra CEO aims to foster EU-style Niemann-Pick market in US
- Chemo-Free Drug, Tecvayli, Shows Major Survival, Remission Gains In Relapsed Multiple Myeloma
- Urine Test Can Detect Autism, Study Says
- High-Puff Vapes Become More Toxic Over Time, Study Says
- Coffee, racetracks, beaches and more coffee—inside the ASCO 2026 exhibit floor
- GLP-1 Drugs Like Ozempic May Lower Breast Cancer Risk By About 30%
- Telehealth Booms As Demand For GLP-1s Surges and Questions Mount About Safety, Oversight
- A patient-first shift in disease language and communication
- Base Case: Remarks at the IC3 Blockchain Camp
- Trump Signs Order Calling For Fewer Childhood Vaccines
- Ascension closes its $3.9B AmSurg purchase following FTC's all-clear
- Simple Blood Test May Help Detect And Stage Alzheimer's Disease
- Smartphone App Helps Those With Advanced Cancer Maintain Quality Of Life
- Asthma Drug, Tezspire, Cuts Need For Steroid Pills While Keeping Attacks In Check
- Childhood Flu Shots Prevent Millions of Cases, Study Finds
- TikTok Videos Fuel Illicit Vaping Culture Among Underage Youth
- Amid Ebola, Hantavirus Outbreaks, Democrats Decry Trump's Health Cuts
- Commission Statement on the Passing of Former General Counsel David Becker
- Your Surprise Medical Bill May Be Gone — But Your Premiums Could Still Spike
- Short-Term Fasting Could Boost Chemo Response in Ovarian Cancer, Study Suggests
- MedTech In Focus: AI impact in healthcare
- If Your AI Can’t Explain Itself, Can FDA Authorize It?
- Workout Habits May Protect Against Inherited Heart Problems
- Childhood Lying Is Normal and Rarely Signals Behavioral Concerns, Study Says
- Perfectionism Among College Students Reaches Record High, Fueling Anxiety
- Climate Change: Statement on Proposed Rescission of Climate-Related Disclosure Rules
- Statement of Commissioner Mark T. Uyeda on the Rescission of Climate-Related Disclosure Rules
- Keynote Remarks at the 2026 Reagan National Economic Forum
- Statement on Proposing Release for Rescission of Climate-Related Disclosure Rules
- Privacy and PetShops: Remarks at the Regulatory PETshop Series: Cryptographic Technologies and Financial Services Regulation
Michigan healthcare freedom community forum
Bridge Michigan magazine has posted a good situation report on the sorry state of Michigan health care which includes some eye watering statistics and numbers:
Michigan health care woes: Insurers leaving, rates rising, subsidies in limbo
By Eli Newman - October 24, 2025* Some major insurers are said to be leaving the state’s Affordable Care Act exchange
* About 530,000 state residents who get their health insurance on the individual market are facing a 16.8% rate hike
* Some analysts estimate 64,000 people in Michigan will go uninsured next yearWith less than two weeks until open enrollment starts, thousands of Michigan residents face a triple challenge.
Not only are premiums going up, but thousands of people who get their health insurance through the Affordable Care Act marketplace may be forced to switch plans because their providers are either fleeing the state’s ACA exchange or scaling back coverage. In addition, it’s uncertain whether enhanced premium subsidies for ACA plans will continue.
About 200,000 individuals may be unable to renew with their current insurer, Joe Sullivan, director of the Office of Innovation and Research at the Michigan Department of Insurance and Financial Services (DIFS), told state lawmakers this week.
Some providers have had to “reevaluate their position” in the state, Sullivan said, amid a federal overhaul of coverage in the Trump era and the ongoing debate over health care subsidies, which are a central issue in the government shutdown.
Members of Congress have been wrangling over a temporary spending plan, and whether it will include an extension of an “enhanced” ACA premium tax credit benefiting millions of Americans.
“The volatility caused by the inaction on enhanced premium tax credits and marketplace reforms have led to a variety of types of withdrawals, including issuers declining to offer certain plan types or remain in certain areas of the state, some withdrawals from just the marketplace or withdrawals from the individual market as a whole,” Sullivan told the Michigan Senate Health Policy Committee on Wednesday.
Hints of Michigan’s changing health care landscape are already appearing on the horizon:
* HAP CareSource notified the state in September it would discontinue its individual marketplace plans for nearly 19,000 enrollees.
* Michigan Medicine is dissolving its UM Health Plan, formerly known as the Physicians Health Plan (PHP), affecting 64,000 enrollees in the Lansing area, citing “significant financial losses over the past few years.”Several health insurance brokers — including Cornerstone, MRW Solutions Group and Agility Insurance Services have warned their Michigan customers of other carriers pulling out. Those said to be scaling back in Michigan include Ambetter Health, from Meridian Health Plan, and Molina Healthcare, which has about 36,000 individuals on the exchange. Neither company immediately responded to Bridge Michigan’s request for comment.
Proposed rate hikes
Whether covered by ACA or an employer, Michigan residents can expect to pay more for health insurance in 2026, according to the rate requests insurers submitted over the summer to the Michigan Department of Insurance and Financial Services.
The state is expected to post approved rates once open enrollment starts on Nov. 1, but projections show nationwide, the average ACA plan will rise by 30%.
Michigan’s health insurance providers requested an average rate hike of 16.8% for the insurance policies sold to individuals, including plans they offer on the ACA marketplace. Those policies cover 530,000 people in Michigan.
In all, 121 of 251 individual plans have a proposed rate hike of 15% or more. One hundred seventy-eight plans, including those provided by Blue Cross Blue Shield of Michigan and Priority Health, will be listed on the ACA health care marketplace.
Small group plans, which cover some 412,000 people working at companies with 50 or fewer employees, are set to see an average rate hike of 11.1%.
Large business plans, which are usually exempt from state insurance mandates, are expecting their largest rate increases in 15 years — 6.5% on average — according to the global consulting firm Mercer.
Sullivan said 90% of state residents who get their plans on the ACA individual market also take advantage of enhanced premium tax credits, saving an average of more than $380 a month.
Those subsidies were temporarily expanded during the COVID-19 emergency and extended in subsequent legislation under the Biden administration, but are slated to expire at the end of the year.
“An estimated 40,000 Michigan families currently enrolled in coverage through HealthCare.gov will no longer receive any premium tax credits,” Sullivan said.
Without an extension, Sullivan said rates are expected to rise for every resident who enrolls in health care coverage.
A ‘double whammy’
Rachel Richards, the fiscal policy director for the Michigan League for Public Policy, told lawmakers in a hearing of the Senate Health Policy Committee this week that households will see a “double whammy” in rate hikes next year — the forecasted rise in costs and the loss of the enhanced premium tax credits.
“A 60-year-old Michigan couple that’s making roughly $82,000 a year would see their annual premiums increase from just shy of $7,000 a year to more than $20,000 a year,” Richards said.
Changes in HR 1, or the One Big Beautiful Bill Act, will also eliminate automatic reenrollment, which Richards says was used by more than half of marketplace users this year.
The resulting changes will result in 108,000 fewer Michiganders being covered on the marketplace next year, according to an analysis from the Urban Institute. The DC-based think tank estimates 64,000 people in the state will go uninsured in 2026.
Michigan’s health insurer lobbyists have joined the chorus of those voicing concerns about the upcoming rate hikes.
“If these tax credits are allowed to expire, the impact will be immediate and severe,” Christine Shearer, deputy director of legislation and advocacy for the Michigan Association of Health Plans, told the committee.
“The potential loss of federal tax credits, combined with rising medical inflation and escalating prescription drug costs could result in some of the steepest premium increases seen in nearly two decades.”
The health plan association is advocating for policy solutions to address the forthcoming changes.
The group says a Basic Health Program, which would provide insurance coverage for individuals just above the Medicaid income threshold could help, along with small business assistance funding, state employee insurance reform and expanding access to association health plans to allow smaller businesses to purchase plans in the large group market.
Bridge Michigan posted a follow up article yesterday specifically addressing the eye watering Michigan health care insurance premium increases.
Unstated in this article: Each and every one of these reasons for skyrocketing premiums were directly caused by the Patient Protection and Affordable Care Act (PPACA), and the follow on Inflation Reduction Act. None will go away until both acts are repealed:
Five reasons health insurance rates are rising so much in Michigan
By Eli Newman - November 5, 2025* Michigan’s insurers have raised individual marketplace rates more than 20% on average for 2026
* Many factors contribute to the rise — market consolidation, expiring government subsidies, drug prices, inflation and hospital costs
* Marketplace and Medicare plans must be selected by Dec. 18 for coverage to begin in JanuaryMichael Steinberg is “petrified” about finding coverage on the individual Affordable Care Act marketplace, where Michigan’s insurers have raised rates more than 20% on average for 2026.
The 62-year-old criminal defense attorney lives in West Bloomfield and needs insurance to cover medication for diabetes and high blood pressure and related doctor visits.
“For me to have an individual health care plan, it’s like over $1,300 a month,” Steinberg told Bridge Michigan, explaining that he has a $4,000 annual deductible for pharmaceuticals and a $7,500 deductible for medical expenses. “It’s egregious.”
Ahead of open enrollment, which started Saturday, Steinberg, along with several Michigan residents, expressed outrage over the planned health insurance rate hikes, drafting letters to the state to voice their concerns.
One woman from Grand Rapids said she’s resorted to donating plasma for money to keep up with payments, all while holding down a full-time job as a state employee. Several people stated their monthly premiums have surpassed what they pay on their home mortgages.
The comments represent the frustrations of a system millions contend with each year.
Michigan residents will need to sign on to new HealthCare.gov plans during open enrollment before Dec. 18 if they want their insurance to take effect at the start of the new year. Others face higher costs for employer-provided and Medicare plans.
Policy analysts and health care stakeholders offer a variety of reasons for the trend — from increasing costs for drugs and hospital care to acts of Congress:
Providers leaving the state
The number of Michigan health insurance providers offering plans that individuals can purchase has dropped steeply.
The state had 41 health insurers offering individual plans in 2011, according to the Government Accountability Office. That number fell to 12 by 2022.
That year, Michigan’s top three health insurers — Blue Cross Blue Shield, Priority Health and Meridian — held 88% of the individual group market share, according to the congressional budgeting office. Large insurers control an even bigger share of employer-provided plans.
While state insurance regulators say the state has historically had a “robust market,” providers are continuing to drop coverage.
“For plan year 2026, Michigan will have 10 issuers in the individual market in 2026, down from 12 in 2025,” Chelsea Lewis, spokesperson for the Michigan Department of Insurance and Financial Services, told Bridge Michigan in an email. “On the Marketplace, Healthcare.gov, Michigan will have 7 issuers, down from 10 in 2025.”
Among the large insurers to remove plans from the ACA exchange next year is Health Alliance Plan (HAP). The company’s president, Margaret Anderson, cited capacity issues among other reasons.
“We would not have the financial resources to keep all of our other lines of business afloat had we decided to stay in the marketplace,” Anderson told Bridge, projecting “significant losses” for next year based on “uncertainties and the increasing cost of marketplace claims, both on a pharmacy and a medical perspective.”
HAP has about 490,000 members today, offering individual plans off-exchange along with commercial and Medicare Advantage coverage.
Congressional analysts say reducing the number of available plans causes premiums to rise, which in turn, “may result in decreased consumer access to affordable health insurance.”
“Although some studies find that concentration can result in reduced costs for issuers … and lower prices paid by issuers to providers for medical care, these savings may not be passed on to consumers as lower premiums,” GAO health care director John Dicken wrote in a 2024 analysis of national private health insurances.
Expiring tax credits
One of the biggest reasons premiums are going up is that insurers are preparing for the end of an enhanced premium tax credit program for health insurance plans bought through HealthCare.gov.
The future of these tax credits lies at the heart of the government shutdown, as lawmakers debate extending the subsidies further. Democrats want assurances that the credits will be extended into the new year and that Medicaid cuts previously approved by President Donald Trump will be reversed. Republicans want to end the shutdown first, holding off on any health care policy negotiation until after a funding bill is approved.
“Congress’s failure to extend the enhanced advanced premium tax credits also contributed to higher rates, as fewer young and/or healthy people are expected to sign up for insurance, which adversely impacts the risk pool,” Lewis said.
Policy analysts estimate 484,000 state residents use the health care subsidy and its expiration may drive people to drop coverage.
“Without the renewal, families will see their monthly premiums skyrocket by more than $400 a month, with some people facing much higher increases,” Monique Stanton, president and CEO of the Michigan League for Public Policy, said during a news conference Tuesday supporting the tax credits.
Stanton said without coverage, patients are more likely to seek medical care at emergency departments, which would raise costs for the overall health care system.
Rising inflation
“Maintaining a facility or purchasing or leasing a space has often gone up in price,” Phillip Bergquist, CEO of the Michigan Primary Care Association, which represents a network of community health clinics across the state, said at the news conference.
The last five years have seen a steep increase in the price of supplies and facility maintenance, Bergquist said, and the “wage competition” for licensed providers and other workers is also on the rise.
“The biggest cost in providing health care is the people who provide the care,” he said.
Bergquist estimates over 22,000 community health center patients will lose coverage statewide as a result of the increase in insurance rates, representing an $18 million reimbursement loss for the clinics providing care.
Hospital costs
Physicians like Dr. Todd Otten of Dimondale partially blame the “out of control” costs on high administrative costs, reflecting an industry where the growth of health care managers has significantly outpaced jobs for doctors.
“There’s a complete disconnect with where the money is going and the outcomes,” Otten said at Tuesday’s public policy news conference.
Insurance executives have blamed ballooning hospital costs for driving premiums up.
According to the Michigan Health Purchasers Coalition, a nonprofit organization to lower costs to employer-sponsored health care plans, 47 cents on the dollar of commercial health plan premiums is spent on hospital services in Michigan.
Bret Jackson, who manages the coalition, is president and CEO of a group of employers and labor union health care advocates known as the Economic Alliance of Michigan. He blames hospital consolidation as the “number one reason” for rising prices.
“This happens everywhere around the country,” Jackson said. “Big, corporate health systems take over and buy more hospitals and buy more doctors and buy more clinics … the prices just inevitably go up because they now have more market power, and they can now demand and get people to pay higher prices for services.”
Michigan’s hospital leaders acknowledge the reality of mergers and acquisitions in the state, but argue that some smaller communities benefit.
“The cost of electronic medical record infrastructure is extraordinary today. The cost of medical liability insurance coverage, the cost of physician practice subsidization,” Brian Peters, CEO of the Michigan Health & Hospital Association, told Bridge. “You’re better able to bear that underlying cost if you’re part of a larger system that has more capital resources.
Peters, who says he’s been lobbying the state’s congressional delegates to extend the enhanced premium tax credits subsidy, worries that “uncompensated care” will force hospitals to lose money.
He said the rise of premiums can be owed to a couple factors outside of congressional gridlock, including the “explosive growth” in drug costs and health care supplies, made worse by federal tariff policy.
Drug prices
Many point to increased post-COVID medical check-ups, increased use of innovative gene therapies and GLP-1 weight loss drugs and pharmaceutical prices outpacing inflation as contributing factors to rising costs.
“As we’re evolving these new therapies and these new advancements, we’re seeing these cost pressures coming in,” HAP’s Anderson said. “Part of insurance is pricing for the risk.”
Dr. Mark Fendrick, who directs the Center for Value-Based Insurance Design at the University of Michigan, said shifting pharmaceutical prices are impacting decisions during Medicare open enrollment, which ends Dec. 7.
“People who have long loved traditional Medicare are moving to Medicare Advantage because they don’t like the fact that their premiums for their drug coverage have gone up,” he said.
Despite consumer sentiment being overly focused on premium price, Fendrick says the monthly expenditure only represents a component of the full financial picture consumers must consider when selecting a plan from Medicare, the individual market or any other private insurer.
“Americans don’t care about health care costs. They care about what it costs them,” Fendrick said. “Premiums are only part of the story.”
Fendrick advises consumers to shop around their plans to check out deductibles and copayments, rather than defaulting on renewing their current coverage, saying they should closely analyze their out-of-pocket exposure before making a decision.
Get MHF Insights
News and tips for your healthcare freedom.
We never spam you. One-step unsubscribe.