- Gounder Fills In Details Behind Ebola, GLP-1, and Trump Headlines
- The rise of the invisible patient experience
- Lifepoint among latest to file underpayment complaint against MultiPlan, insurers
- Untreated Cancer, Festering Infections: Immigrant Detainees Detail Medical Care Lapses
- Virginia dental practice suffers data breach affecting 5,200 individuals
- CRNAs could gain foothold in Medicare payment models
- Virginia oral surgery practice suffers data breach affecting 7,000 individuals
- 3 cases redrawing the lines of physician contracting
- 13 recent health system CIO moves
- ‘IDR is the exception, not the rule’: TeamHealth CMO on billing reality
- Judge blocks Munson Healthcare’s bid to transfer Oracle Health data breach lawsuits
- States ranked by mental health social workers per capita
- Nebraska hospital names CEO
- 46 recent hospital, health system executive moves
- When nurses work 2 jobs, no one tracks the total hours
- Minnesota system promotes COO to CEO
- Ascension Via Christi taps new CEO from HCA
- Wellstar to acquire 25-bed critical access hospital: 4 things to know
- UnitedHealthcare cut CRNA pay 15% — are ASCs picking up the tab?
- Waco Cardiology’s research arm acquired in 3-city deal
- New York opens 60-bed OUD recovery center
- Kratom admissions jump 525% at California treatment center
- Buy, join or partner? Dentists’ advice for new grads
- The 10 states where ophthalmologists’ pay climbed the most
- Addiction Recovery Care founder indicted on fraud, money laundering charges
- Dengue Is No Longer Just A Travel Risk — What Google’s Mosquito Plan Could Mean For Your Summer
- Catholic Health acquires majority stake in ASC
- Ohio targets behavioral health fraud with new oversight measures
- 12 state behavioral health policy updates
- California dental practice adds humanoid robot for front-desk help
- What happened to the nerve block coverage denial? Where the fight stands now
- DentaQuest cybersecurity incident exposes 2.6 million accounts
- U of Colorado partnership to accelerate inflammatory bowel research
- UC Davis, California endoscopy center to launch GI fellowship
- The 5 states with the most DSO action in May
- 5 highest-paying cities for dental assistants in 2026
- 5 highest-paying cities for hygienists in 2026
- 3 dental acquisitions in May
- 7 DSOs making headlines
- Brain Surgery For Pituitary Tumor Helps Illinois Mom Have Second Baby
- Takeda takes $2.5B legal charge after pay-for-delay verdict, swings to loss for '25
- Industry Voices—A healthcare experience that is as seamless as it is soulful
- Fullspan Health debuts Healthline AI companion to connect consumers to medical content and providers
- As pro-life pressure ramps up on Trump, FDA is investigating safety of abortion pill: WSJ
- As pro-life pressure ramps up on Trump, FDA is investigating safety of abortion pill: WSJ
- Popular Blood Pressure Meds, Dihydropyridine Calcium-Channel Blockers, Linked To Kidney Damage Risk In Type 2 Diabetes
- Too Much Sitting In Pregnancy Doubles Risk Of Complications
- Spinal Cord Stimulation May Restore Arm Strength After Stroke
- Behind the headlines of ASCO 2026
- RFK Jr. Seeks To Peek At Americans' Medical Records For Clues On Autism And Vaccines
- Two-Pill Combo, Inqovi and Venclexta, Offers Hospital-Free Leukemia Treatment Option For Older Adults With AML
- ‘We Live With Fear’: In Congo, Doctors Face Ebola With Little Protection
- Millions of Kids Could Lose Insurance as GOP Healthcare Cuts Start To Bite
- Upcoming Billing Change Could Make Pregnancy Pricier
- WellSpan Health strikes strategic partnership with Philips to deploy, co-develop new healthcare tech
- Oregon overhauls 30-year behavioral health agreement model: 3 things to know
- 6 states regulating AI in mental health
- RWJBarnabas Health sets 15K target for naloxone kit program
- 4 charged in $30M behavioral health fraud case
- At first public hearing for FDA’s CNPV program, industry support meets ‘deep concern’ from experts
- “Harmonization: We’ll Have Lots to Talk About”
- Remarks at the Investor Advisory Committee Meeting
- A Quarter for your Thoughts: Remarks at the Meeting of the SEC Investor Advisory Committee
- Weekly Rundown: Trump signs AI executive order; Health Catalyst to sell Vitalware for $147M
- Small businesses feel the squeeze as healthcare costs rise: Morgan Health
- Poll Finds Broad Support For Stricter Regulations On Ultra-Processed Foods
- It's unanimous: SCOTUS agrees with Hikma in 'skinny label' case vs. Amarin
- Remarks at the Investor Advisory Committee Meeting
- Fierce Pharma Asia—China's biotech rise; ASCO highlights; Lilly pipeline deals
- Nearly 1 in 5 Young People Turn to AI Chatbots for Mental Health Advice
- Ixlayer rolls out digital acute pain management platform in collaboration with Vertex Pharmaceuticals
- Georgetown study: 2M children have dropped out of Medicaid, CHIP since January 2025
- ScionHealth sends 8 community hospitals to Lifepoint Health
- ADC Therapeutics' shares plummet after patient deaths in trial of Zynlonta
- As China biotech crackdown calls reverberate in Washington, the pushback gets louder, too
- Older LGBTQ+ Adults Fear Less Support As They Age, Poll Shows
- Night Owls Are More Prone To Anxiety, Loneliness
- Home-Delivered Medical Meals Reduce ER Visits, Save Money
- Axsome fends off generic competition to narcolepsy med Sunosi until 2040
- Menopause Hormone Therapy Use Drops Sharply Across United States
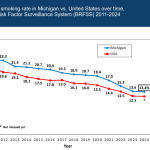
- Michigan Found A Way To Reduce School Vaccine Waivers — Until It Backfired
- Listen to the Latest ‘KFF Health News Minute’
- RFK Jr. Seeks To Peek at Americans’ Medical Records for Clues on Autism and Vaccines
- Louisiana’s Reporting Law Chills Immigrant Medicaid Applications
- Thyme Care expands cancer survivorship program to provide longitudinal support
- Medline earns FDA warning letter ire for repeated toxic bacteria problems
- Trump’s Medicaid Work Rules Force States To Scrap Plans and Rework Systems
- Commonwealth Fund: 21% of adults experienced a coverage denial in the past year
- Healthcare Dealmakers—WakeMed to join Atrium Health, Qualtrics closes $6.8B Press Ganey deal and more
- Millions on Medicaid May Soon Have To Prove They’re Working To Keep Coverage
- Anomaly Insights launches AI solution for managed care executives
- Lilly, Boehringer to slash at least $1B each from planned investments in Germany
- Presbyterian Healthcare Services to discontinue MA plans in 2027, cut 150 jobs
- Just 90 Minutes Of Strength Training A Week Linked To Longer Life
- AHA lays out blueprint to improve affordability, care access and quality
- Amid Miplyffa launch, Zevra CEO aims to foster EU-style Niemann-Pick market in US
- Chemo-Free Drug, Tecvayli, Shows Major Survival, Remission Gains In Relapsed Multiple Myeloma
- Urine Test Can Detect Autism, Study Says
- High-Puff Vapes Become More Toxic Over Time, Study Says
- With Cencora pact, Gilead looks to grow CAR-T treatment center network
- The watchdog overseeing the integrity of HHS programs
- Coffee, racetracks, beaches and more coffee—inside the ASCO 2026 exhibit floor
- GLP-1 Drugs Like Ozempic May Lower Breast Cancer Risk By About 30%
- Telehealth Booms As Demand For GLP-1s Surges and Questions Mount About Safety, Oversight
- Michigan Found a Way To Reduce School Vaccine Waivers. Until It Backfired.
- A patient-first shift in disease language and communication
- FDA issues untitled letter after finding ‘eye-catching graphics’ in promotional emails
- Neurotech launches new YouTube channel to spotlight patients’ stories for rare eye disorder
- As Akeso takes center stage at ASCO, China biotech industry cements its coming of age
- Base Case: Remarks at the IC3 Blockchain Camp
- Microsoft, Mayo Clinic plan to build frontier AI model for healthcare
- Department of Labor's proposed foreign worker wage increases are more tough news for healthcare staffing
- Trump Signs Order Calling For Fewer Childhood Vaccines
- Industry groups say final Medicaid work requirements rule imposes onerous documentation burden
- Ascension closes its $3.9B AmSurg purchase following FTC's all-clear
- Simple Blood Test May Help Detect And Stage Alzheimer's Disease
- Eli Lilly's ultimatum to hospitals: Send 340B claims data by June 8 or lose discounts
- Marilyn Monroe and Amy Schumer profiled in endometriosis awareness push
- Merck shrinks headcount by 88 in New Jersey as $3B cost-cutting scheme advances
- Gilead's Livdelzi scores in rare liver disease trial, portending use in broader patient population
- Smartphone App Helps Those With Advanced Cancer Maintain Quality Of Life
- Asthma Drug, Tezspire, Cuts Need For Steroid Pills While Keeping Attacks In Check
- Childhood Flu Shots Prevent Millions of Cases, Study Finds
- Amid Ebola, Hantavirus Outbreaks, Democrats Decry Trump's Health Cuts
- TikTok Videos Fuel Illicit Vaping Culture Among Underage Youth
- Commission Statement on the Passing of Former General Counsel David Becker
- Your Surprise Medical Bill May Be Gone — But Your Premiums Could Still Spike
- Athenahealth rolls out over 80 new, expanded AI RCM features in ‘roadmap’ on athenaOne platform
- Short-Term Fasting Could Boost Chemo Response in Ovarian Cancer, Study Suggests
- MedTech In Focus: AI impact in healthcare
- If Your AI Can’t Explain Itself, Can FDA Authorize It?
- Workout Habits May Protect Against Inherited Heart Problems
- Childhood Lying Is Normal and Rarely Signals Behavioral Concerns, Study Says
- Perfectionism Among College Students Reaches Record High, Fueling Anxiety
- After Her Bout of Amnesia, A $59,000 Billing Dispute Wouldn't Go Away
- Weed Linked To Higher Testosterone Levels In Young Men
- Rising Stars: WPP’s Meghan O’Hora on the ‘complex puzzle’ of oncology drug marketing
- Contraception For Teens: Let's Talk About It
- Climate Change: Statement on Proposed Rescission of Climate-Related Disclosure Rules
- Kenyan Court Blocks Trump's Plan To Quarantine Ebola Patients
- Statement of Commissioner Mark T. Uyeda on the Rescission of Climate-Related Disclosure Rules
- Keynote Remarks at the 2026 Reagan National Economic Forum
- Statement on Proposing Release for Rescission of Climate-Related Disclosure Rules
- Mental Health Disorders Now No. 1 Cause of Disability Worldwide
- Study: LA Canine Outbreak Caused By Low Vaccination Rates, Crowded Boarding
- Ocrelizumab Effective In Slowing Progressive MS, Trial Shows
- Privacy and PetShops: Remarks at the Regulatory PETshop Series: Cryptographic Technologies and Financial Services Regulation
- CAT on a Hot Tin Roof
- Remarks at the Stanford Rock Center for Corporate Governance
- Fixing Eligibility at the Point of Care: The Missing Link in Medical Device Reimbursement Integrity
Michigan healthcare freedom community forum
Sen. Stephanie Chang introduced Senate Bill 922 to require private insurers to cover
(a) Fertility diagnostic care.
(b) Fertility treatment.
(c) Standard fertility preservation services.
(d) At least 4 complete oocyte retrievals with unlimited embryo transfers from those oocyte retrievals or from any oocyte retrieval.
(e) The medical costs related to an embryo transfer to be made from or on behalf of an insured to a third party. However, the insured's coverage must not extend to any medical costs of a surrogate after the embryo transfer.
(f) Coverage regardless of whether donor gametes or embryos are used or if an embryo will be transferred to a surrogate.
Copays are expressly forbidden, so expect these expensive treatments to drive up your premiums if SB 922 passes. SB 922 was referred to the Senate Committee on Finance, Insurance, and Consumer Protection:
https://www.legislature.mi.gov/documents/2025-2026/billintroduced/Senate/htm/2026-SIB-0922.htm
SENATE BILL NO. 922
April 23, 2026, Introduced by Senators CHANG, IRWIN, MCMORROW, BAYER, CAVANAGH, SINGH, MOSS, GEISS, CAMILLERI, POLEHANKI, KLINEFELT and CHERRY and referred to Committee on Finance, Insurance, and Consumer Protection. - Title: Intro, sponsors, and referral
A bill to amend 1956 PA 218, entitled
"The insurance code of 1956,"
(MCL 500.100 to 500.8302) by adding section 3406cc.
the people of the state of michigan enact:
Sec. 3406cc. (1) Beginning January 1, 2027, an insurer that delivers, issues for delivery, or renews in this state a health insurance policy shall provide coverage for the treatment of infertility, including all of the following:
(a) Fertility diagnostic care.
(b) Fertility treatment.
(c) Standard fertility preservation services.
(d) At least 4 complete oocyte retrievals with unlimited embryo transfers from those oocyte retrievals or from any oocyte retrieval.
(e) The medical costs related to an embryo transfer to be made from or on behalf of an insured to a third party. However, the insured's coverage must not extend to any medical costs of a surrogate after the embryo transfer.
(f) Coverage regardless of whether donor gametes or embryos are used or if an embryo will be transferred to a surrogate.
(2) Coverage for the treatment of infertility under this section must be provided without discrimination on the basis of age, ancestry, disability, domestic partner status, gender, gender expression, gender identity, genetic information, marital status, national origin, race, religion, sex, or sexual orientation.
(3) An insurer described in subsection (1) shall not impose any of the following:
(a) Deductibles, copayments, coinsurance, benefit maximums, waiting periods, or any other limitations on coverage for the diagnosis and treatment of infertility, including the prescription of fertility medications, different from those imposed on benefits for services not related to infertility.
(b) Preexisting condition exclusions or preexisting condition waiting periods on coverage for the diagnosis and treatment of infertility or the use of any prior diagnosis, an individual's disability, or prior treatment for infertility as a basis for excluding, limiting, or otherwise restricting the availability of coverage for required benefits.
(c) Limitations on coverage based solely on arbitrary factors, including number of attempts, dollar amounts, or age, or providing different benefits to, or impose different requirements on, a class protected under the Elliot-Larsen civil rights act, 1976 PA 453, MCL 37.2101 to 37.2804, than that provided to other insureds.
(d) Exclusions, limitations, or other restrictions on coverage of fertility medications that are different from those imposed on any other prescription medications.
(e) Limitations under the policy based on anything other than the medical assessment of an individual's licensed health care provider.
(4) An insurer described in subsection (1) shall provide coverage under this section regardless of whether the insured foregoes a particular fertility treatment or procedure if the insured's health care provider determines that the treatment or procedure is likely to be unsuccessful or the insured seeks to use previously retrieved oocytes or embryos.
(5) As used in this section:
(a) "Fertility diagnostic care" means procedures, products, genetic testing, medications, counseling, and services intended to provide information and counseling about an individual's fertility, including laboratory assessments and imaging studies.
(b) "Fertility treatment" means procedures, products, genetic testing, medications, counseling, and services intended to establish a pregnancy or treat infertility and that are provided in a manner consistent with established medical practice and professional guidelines published by the American Society for Reproductive Medicine.
(c) "Gamete" means sperm or egg.
(d) "Health care provider" means any of the following:
(i) Nurse practitioner. As used in this subparagraph, "nurse practitioner" means an individual who is licensed as a registered professional nurse under part 172 of the public health code, 1978 PA 368, MCL 333.17201 to 333.17242, who has been granted a specialty certification as a nurse practitioner by the Michigan board of nursing under section 17210 of the public health code, 1978 PA 368, MCL 333.17210.
(ii) Physician.
(iii) Physician's assistant. As used in this subparagraph, "physician's assistant" means an individual who is licensed to engage in the practice as a physician's assistant under part 170, 175, or 180 of the public health code, 1978 PA 368, MCL 333.17001 to 333.17097, 333.17501 to 333.17556, and 333.18001 to 333.18058.
(e) "Infertility" means any of the following:
(i) The presence of a condition recognized by a health care provider that impacts an individual's ability to establish a pregnancy or to carry a pregnancy. This includes infertility arising from disabilities or from medical treatments or conditions associated with disability.
(ii) An individual's inability to establish pregnancy as an individual or with a partner because the individual or the individual and the individual's partner do not have the necessary gametes to establish a pregnancy.
(iii) An individual's inability to establish a pregnancy or to carry a pregnancy to live birth after 12 months of unprotected sexual intercourse when the individual and the individual's partner have the necessary gametes to establish pregnancy. Pregnancy loss does not restart the 12-month period.
(iv) An individual's inability to establish pregnancy after 6 months of unprotected sexual intercourse due to the individual's age when the individual and the individual's partner have the necessary gametes to establish pregnancy, or to carry a pregnancy to live birth. Pregnancy loss does not restart the 6-month period.
(f) "Oocyte" means an ovum or egg cell before maturation.
(g) "Physician" means either of the following:
(i) A physician licensed to engage in the practice of medicine under part 170 of the public health code, 1978 PA 368, MCL 333.17001 to 333.17097.
(ii) A physician licensed to engage in the practice of osteopathic medicine and surgery under part 175 of the public health code, 1978 PA 368, MCL 333.17501 to 333.17556.
(h) "Standard fertility preservation services" means procedures, products, genetic testing, medications, counseling, and services intended to preserve fertility, consistent with established medical practice and professional guidelines published by the American Society for Reproductive Medicine, or the American Society for Clinical Oncology for an individual who has a medical or genetic condition, including conditions related to disability or chronic illness, or who is expected to receive medical treatment that has a side effect or possible side effect of a risk to an individual's fertility and includes, but is not limited to, expenses related to evaluation, laboratory assessments, medications, and treatment, as well as the procurement and cryopreservation of gametes, embryos, and reproductive material and storage.
Get MHF Insights
News and tips for your healthcare freedom.
We never spam you. One-step unsubscribe.