- Millions of Kids Could Lose Insurance as GOP Healthcare Cuts Start To Bite
- ‘We Live With Fear’: In Congo, Doctors Face Ebola With Little Protection
- Upcoming Billing Change Could Make Pregnancy Pricier
- Oregon overhauls 30-year behavioral health agreement model: 3 things to know
- Broward hospital taps chief medical officer from Sentara
- Anthropic pushes for a frontier AI pause
- Novant Health saves 1,595 inpatient bed days with hospital at home
- Do hospital rankings improve care — or just chase scores?
- 6 states regulating AI in mental health
- HHS cuts funds for Hawaii’s Medicaid fraud unit
- Health systems welcome Anthropic cybersecurity collaboration
- Why the most successful practices are reimagining the hygienist role
- Park Dental Partners adds Minnesota practice
- Medicaid work rules: What’s in, what’s out and where hospitals stand
- Med-Metrix to acquire Vitalware from Health Catalyst
- 850 Virtua nurses issue strike notice
- What leaders need to know about the breakthrough pancreatic cancer pill
- Ascension’s $3.9B AmSurg deal signals a new ASC antitrust era — here’s how leaders are responding
- RWJBarnabas Health sets 15K target for naloxone kit program
- The MVP for ASCs in payer negotiations
- Aspen Dental opens Missouri practice
- 3 dental technologies earning FDA clearance
- Fraud crackdown heats up: 9 physicians in 60 days
- Optum to close another Indiana physician practice
- Closures, bankruptcies and consent orders: 5 ASC controversies from the last year
- The No Surprises Act’s game of ‘hot potato’
- New Maryland law expands assignment of benefit protections for dentists, patients
- Insurers overturn 80% of denied IBD therapy claims on appeal — but only 4% are ever challenged
- Rhode Island House passes bill expanding reimbursement options for hygienists: 5 notes
- Dental assistants’ pay jumped the most in these 10 states
- 4 charged in $30M behavioral health fraud case
- Medicaid termination notices disrupt South Florida behavioral healthcare
- Cooper University Health Care plans $300M ASC, outpatient campus
- “Harmonization: We’ll Have Lots to Talk About”
- HUD overhauls $4B homelessness program
- Heartland Dental added 8 practices in May
- What the USAP-FTC settlement means for ASC anesthesia contracting
- 15 spine surgeons to know
- PDS Health marks $1M in tuition assistance for dental assisting students
- Remarks at the Investor Advisory Committee Meeting
- A Quarter for your Thoughts: Remarks at the Meeting of the SEC Investor Advisory Committee
- 5 highest-paying cities for dentists in 2026
- ‘The need has not magically decreased’: John Muir temporarily closes 21 psych beds amid California’s staffing order
- Small businesses feel the squeeze as healthcare costs rise: Morgan Health
- Poll Finds Broad Support For Stricter Regulations On Ultra-Processed Foods
- It's unanimous: SCOTUS agrees with Hikma in 'skinny label' case vs. Amarin
- Remarks at the Investor Advisory Committee Meeting
- Nearly 1 in 5 Young People Turn to AI Chatbots for Mental Health Advice
- Ixlayer rolls out digital acute pain management platform in collaboration with Vertex Pharmaceuticals
- Georgetown study: 2M children have dropped out of Medicaid, CHIP since January 2025
- ScionHealth sends 8 community hospitals to Lifepoint Health
- ADC Therapeutics' shares plummet after patient deaths in trial of Zynlonta
- As China biotech crackdown calls reverberate in Washington, the pushback gets louder, too
- Older LGBTQ+ Adults Fear Less Support As They Age, Poll Shows
- Night Owls Are More Prone To Anxiety, Loneliness
- Home-Delivered Medical Meals Reduce ER Visits, Save Money
- Axsome fends off generic competition to narcolepsy med Sunosi until 2040
- Menopause Hormone Therapy Use Drops Sharply Across United States
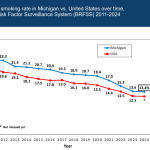
- Michigan Found A Way To Reduce School Vaccine Waivers — Until It Backfired
- Listen to the Latest ‘KFF Health News Minute’
- Louisiana’s Reporting Law Chills Immigrant Medicaid Applications
- RFK Jr. Seeks To Peek at Americans’ Medical Records for Clues on Autism and Vaccines
- Thyme Care expands cancer survivorship program to provide longitudinal support
- Medline earns FDA warning letter ire for repeated toxic bacteria problems
- Michigan psychiatric hospitals cut patient injuries 58%
- 28 behavioral health executive moves to know
- Carilion behavioral health role cuts staff injuries 70%-90%
- Trump’s Medicaid Work Rules Force States To Scrap Plans and Rework Systems
- Commonwealth Fund: 21% of adults experienced a coverage denial in the past year
- Millions on Medicaid May Soon Have To Prove They’re Working To Keep Coverage
- Anomaly Insights launches AI solution for managed care executives
- Lilly, Boehringer to slash at least $1B each from planned investments in Germany
- Presbyterian Healthcare Services to discontinue MA plans in 2027, cut 150 jobs
- Just 90 Minutes Of Strength Training A Week Linked To Longer Life
- AHA lays out blueprint to improve affordability, care access and quality
- Amid Miplyffa launch, Zevra CEO aims to foster EU-style Niemann-Pick market in US
- Chemo-Free Drug, Tecvayli, Shows Major Survival, Remission Gains In Relapsed Multiple Myeloma
- Urine Test Can Detect Autism, Study Says
- High-Puff Vapes Become More Toxic Over Time, Study Says
- With Cencora pact, Gilead looks to grow CAR-T treatment center network
- The watchdog overseeing the integrity of HHS programs
- Coffee, racetracks, beaches and more coffee—inside the ASCO 2026 exhibit floor
- GLP-1 Drugs Like Ozempic May Lower Breast Cancer Risk By About 30%
- Telehealth Booms As Demand For GLP-1s Surges and Questions Mount About Safety, Oversight
- At a Tennessee Hospital, a Nurse Stole Fentanyl and AI Missed It, State Records Say
- Michigan Found a Way To Reduce School Vaccine Waivers. Until It Backfired.
- A patient-first shift in disease language and communication
- FDA issues untitled letter after finding ‘eye-catching graphics’ in promotional emails
- Neurotech launches new YouTube channel to spotlight patients’ stories for rare eye disorder
- As Akeso takes center stage at ASCO, China biotech industry cements its coming of age
- Base Case: Remarks at the IC3 Blockchain Camp
- Microsoft, Mayo Clinic plan to build frontier AI model for healthcare
- OIG: Feds may have overpaid MA plans by millions due to unsupported stroke diagnoses
- Department of Labor's proposed foreign worker wage increases are more tough news for healthcare staffing
- Trump Signs Order Calling For Fewer Childhood Vaccines
- Industry groups say final Medicaid work requirements rule imposes onerous documentation burden
- Ascension closes its $3.9B AmSurg purchase following FTC's all-clear
- Simple Blood Test May Help Detect And Stage Alzheimer's Disease
- Festering Infections to Untreated Cancer: ICE Detainees Describe Medical Neglect Across US
- A look at wearable adoption trends and who's using 'smart' devices: Rock Health
- Eli Lilly's ultimatum to hospitals: Send 340B claims data by June 8 or lose discounts
- Eli Lilly's ultimatum to hospitals: Send 340B claims data by June 8 or lose discounts
- Marilyn Monroe and Amy Schumer profiled in endometriosis awareness push
- Merck shrinks headcount by 88 in New Jersey as $3B cost-cutting scheme advances
- Joint Commission launches voluntary AI certification program for healthcare organizations
- Gilead's Livdelzi scores in rare liver disease trial, portending use in broader patient population
- Smartphone App Helps Those With Advanced Cancer Maintain Quality Of Life
- Asthma Drug, Tezspire, Cuts Need For Steroid Pills While Keeping Attacks In Check
- Childhood Flu Shots Prevent Millions of Cases, Study Finds
- Sanofi taps Snowflake for AI field agent help
- Merck weighs use of COVID antiviral Lagevrio as Ebola outbreak worsens
- ADHD drug delivery specialist Cingulate hit with manufacturing-related FDA rejection
- Amid Ebola, Hantavirus Outbreaks, Democrats Decry Trump's Health Cuts
- TikTok Videos Fuel Illicit Vaping Culture Among Underage Youth
- Eisai whips up Alzheimer’s dietary guidance to expand nutrition program beyond cancer
- Northwell's firearm injury risk screener now widely available within Epic
- Commission Statement on the Passing of Former General Counsel David Becker
- Your Surprise Medical Bill May Be Gone — But Your Premiums Could Still Spike
- Athenahealth rolls out over 80 new, expanded AI RCM features in ‘roadmap’ on athenaOne platform
- Contraline and its male birth control candidate rally $92.5M amid push into 'massive white space' of men's health
- Short-Term Fasting Could Boost Chemo Response in Ovarian Cancer, Study Suggests
- MedTech In Focus: AI impact in healthcare
- If Your AI Can’t Explain Itself, Can FDA Authorize It?
- Wolters Kluwer Health survey examines AI use and concerns among clinicians, patients in 2026
- Workout Habits May Protect Against Inherited Heart Problems
- Childhood Lying Is Normal and Rarely Signals Behavioral Concerns, Study Says
- Perfectionism Among College Students Reaches Record High, Fueling Anxiety
- After Her Bout of Amnesia, A $59,000 Billing Dispute Wouldn't Go Away
- Weed Linked To Higher Testosterone Levels In Young Men
- Rising Stars: WPP’s Meghan O’Hora on the ‘complex puzzle’ of oncology drug marketing
- Contraception For Teens: Let's Talk About It
- Climate Change: Statement on Proposed Rescission of Climate-Related Disclosure Rules
- Kenyan Court Blocks Trump's Plan To Quarantine Ebola Patients
- Statement of Commissioner Mark T. Uyeda on the Rescission of Climate-Related Disclosure Rules
- Keynote Remarks at the 2026 Reagan National Economic Forum
- Statement on Proposing Release for Rescission of Climate-Related Disclosure Rules
- Mental Health Disorders Now No. 1 Cause of Disability Worldwide
- Study: LA Canine Outbreak Caused By Low Vaccination Rates, Crowded Boarding
- Ocrelizumab Effective In Slowing Progressive MS, Trial Shows
- Long COVID Might Be Twice As Common As Previously Thought
- In Vaccine-Skeptical California County, A Potential Playbook To Contain Measles
- Heavy Drinking Harms College Students' Brain Power, Study Finds
- Bangladesh Measles Surge Kills 500+ Children; Vaccine Delays Blamed
- Plant-Based Diet May Cut Obesity Risk For Women In Menopause
- Smartwatch App Accurately Detects Major Epileptic Seizures
- Racial Gap Exists For Asthma Inhaler Use
- Privacy and PetShops: Remarks at the Regulatory PETshop Series: Cryptographic Technologies and Financial Services Regulation
- CAT on a Hot Tin Roof
- Remarks at the Stanford Rock Center for Corporate Governance
- Fixing Eligibility at the Point of Care: The Missing Link in Medical Device Reimbursement Integrity
Michigan healthcare freedom community forum
The Veteran's Health Care Act (P.L. 102-585) (now Section 340B(a)(4) of the Public Health Service Act) "340B" drug pricing program is very popular amongst nonprofit hospitals and Democratic legislators because it forces huge discounts on Big Pharma. The Michigan Senate passed SB 94 back in March which will mandate drug suppliers' continued participation in the 340B program, if passed into law.
There are many problems with 340B, and one stands out here in Michigan. The 340B discounts cut Big Pharma's top line, transferring their profits to supposedly nonprofit hospitals. This reduces the corporate income tax proceeds from Michigan-based pharmaceutical companies like Pfizer. Nonprofit hospitals pay no corporate income taxes, so the State of Michigan loses that revenue completely:
A 'Free' Federal Program Is Blowing a Hole in State Budgets
By Dan Crippen - July 11, 2025An obscure, supposedly free federal program is quietly blowing a hole in state budgets -- by depriving state governments of billions in corporate tax revenue and inflating costs for their public employee health plans.
The culprit is the 340B Drug Pricing Program, which Congress established in 1992 to help safety-net hospitals. Once enrolled in the program, qualifying hospitals and clinics and their partner pharmacies -- collectively called "covered entities" -- can purchase medicines directly from drug manufacturers or wholesalers at roughly 50% discounts.
In the program's first year, just 50 hospitals enrolled. And as I documented in a recent white paper, Congress expected only about 90 hospitals to ultimately participate. But today, more than 2,600 hospitals are enrolled.
This explosive, albeit unintended, growth is the result of the program's lax requirements. Covered entities are not required to expand charity care, or even report how they use their 340B earnings.
Hospitals ultimately realized they could buy heavily discounted drugs and then resell them to insured, middle-class patients at huge markups. In some cases, hospitals have charged cancer patients nearly ten times what they paid to acquire the drug.
The opportunity to upcharge patients has proven irresistible -- and fueled the program's bloat. Total purchases through the program have soared 129% just from 2018 to 2023, more than triple the growth in drug purchases outside the program during that time. In 2023, covered entities purchased over $124 billion worth of medicines when priced at wholesale acquisition cost -- but only actually paid $66 billion, meaning they received roughly $58 billion in discounts on those drugs.
Numerous audits and investigations have revealed that many hospitals use the funds to subsidize expansion in affluent neighborhoods, rather than to support low-income or uninsured patients. Even at "disproportionate share" hospitals -- facilities that supposedly are safety-net providers -- less than half of 340B earnings go toward charity care.
This perverse behavior directly harms state taxpayers.
Because most 340B hospitals are technically non-profits, their earnings aren't taxed. The program effectively transfers $70 billion -- the $58 billion in discounted purchases, plus other discounts that result from the interplay of 340B with other programs -- from for-profit drug companies to mostly non-profit hospitals, clinics, and other covered entities.
As a result, states collect about $3.5 billion less in corporate income tax and other tax revenue from drug companies than they otherwise would. That's money not available for public health, education, infrastructure, or employee benefits.
The 340B program hurts states in other ways, too.
Consider how the program incentivizes hospital systems to acquire previously independent clinics -- which don't qualify for 340B -- and designate them as "child sites" that subsequently become eligible for 340B. A study in the New England Journal of Medicine found that 340B has "induced provider consolidation" and consequently resulted in "more hospital-based administration" of drugs, rather than clinic-based administration.
This, in turn, leads to higher healthcare spending, since care provided at hospital-owned sites is generally more expensive than care at clinics and independent practices.
In fact, care at 340B hospitals tends to be more expensive than care at competing hospitals too. The average per-patient prescription spending at 340B hospitals is roughly 150% higher than non-340B hospitals, according to a Milliman analysis.
That's partly because enrolled hospitals have a greater incentive "to prescribe brand drugs where the potential profit from 340B is greater than for generic drugs," as one Columbia University professor put it.
All told, large employers -- ones that "self-insure" their own health benefits -- and their workers spend over $5 billion more per year on health care as a result of 340B. Every extra dollar that businesses spend on health care is a dollar that's deducted from their taxable income.
The program also directly inflates costs for state employee health plans. Utah recently found that its Public Employees Health Program -- the insurance plan for roughly 160,000 state and local government employees -- is losing out on $3.9 million in rebate savings due to 340B.
Yet some state lawmakers are unwittingly compounding the damage -- by making it easier for pharmacies not currently enrolled in the program to contract with 340B hospitals and clinics. Utah recently enacted such a bill, despite the legislature's own study warning that if every pharmacy became eligible for the program, the state health plan would lose $14.6 million. Even a 10% increase in drugs prescribed through 340B would cost the plan an additional $1.9 million.
More populous states would obviously face much higher losses. For instance, imagine if California -- which already revamped its Medicaid program to minimize 340B losses -- were to similarly expand pharmacies' ability to contract with 340B enrollees. Its CALPERS health plan, which covers 1.5 million current and retired public employees, could easily lose tens, or perhaps even hundreds, of millions of dollars annually, depending on the number of pharmacies that join.
Instead of boosting charity care for poor patients, 340B drains public resources while enriching large hospital systems. Reform is desperately needed.
Dan Crippen is the former Director of the Congressional Budget Office. Dan is from Canistota, South Dakota.
Get MHF Insights
News and tips for your healthcare freedom.
We never spam you. One-step unsubscribe.